Proof-of-principle evaluation of the efficacy of fewer than three doses of a bivalent HPV16/18 vaccine
- PMID: 21908768
- PMCID: PMC3186781
- DOI: 10.1093/jnci/djr319
Proof-of-principle evaluation of the efficacy of fewer than three doses of a bivalent HPV16/18 vaccine
Abstract
Background: Three-dose regimens for human papillomavirus (HPV) vaccines are expensive and difficult to complete, especially in settings where the need for cervical cancer prevention is greatest.
Methods: We evaluated the vaccine efficacy of fewer than three doses of the HPV16/18 vaccine Cervarix in our Costa Rica Vaccine Trial. Women were randomly assigned to receive three doses of the HPV16/18 vaccine or to a control vaccine and were followed for incident HPV16 or HPV18 infection that persisted in visits that were 10 or more months apart (median follow-up 4.2 years). After excluding women who had no follow-up or who were HPV16 and HPV18 DNA positive at enrollment, 5967 women received three vaccine doses (2957 HPV vaccine vs 3010 control vaccine), 802 received two doses (422 HPV vs. 380 control), and 384 received one dose (196 HPV vs. 188 control). Reasons for receiving fewer doses and other pre- and post-randomization characteristics were balanced within each dosage group between women receiving the HPV and control vaccines.
Results: Incident HPV16 or HPV18 infections that persisted for 1 year were unrelated to dosage of the control vaccine. Vaccine efficacy was 80.9% for three doses of the HPV vaccine (95% confidence interval [CI] = 71.1% to 87.7%; 25 and 133 events in the HPV and control arms, respectively), 84.1% for two doses (95% CI = 50.2% to 96.3%; 3 and 17 events), and 100% for one dose (95% CI = 66.5% to 100%; 0 and 10 events).
Conclusion: Four years after vaccination of women who appeared to be uninfected, this nonrandomized analysis suggests that two doses of the HPV16/18 vaccine, and maybe even one dose, are as protective as three doses.
Figures
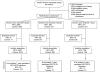
Comment in
-
Less is more: a step in the right direction for human papillomavirus (HPV) vaccine implementation.J Natl Cancer Inst. 2011 Oct 5;103(19):1424-5. doi: 10.1093/jnci/djr354. Epub 2011 Sep 9. J Natl Cancer Inst. 2011. PMID: 21908769 No abstract available.
References
-
- Ferlay J, Shin HR, Bray F, Forman D, Mathers C, Parkin DM. Estimates of worldwide burden of cancer in 2008: GLOBOCAN 2008. Int J Cancer. 2010;127(12):2893–2917. - PubMed
-
- Paavonen J, Naud P, Salmeron J, et al. Efficacy of human papillomavirus (HPV)-16/18 AS04-adjuvanted vaccine against cervical infection and precancer caused by oncogenic HPV types (PATRICIA): final analysis of a double-blind, randomised study in young women. Lancet. 2009;374(9686):301–314. - PubMed
-
- FUTURE II Study Group. Quadrivalent vaccine against human papillomavirus to prevent high-grade cervical lesions. N Engl J Med. 2007;356(19):1915–1927. - PubMed
-
- Goldie SJ, O’Shea M, Diaz M, Kim SY. Benefits, cost requirements and cost-effectiveness of the HPV16,18 vaccine for cervical cancer prevention in developing countries: policy implications. Reprod Health Matters. 2008;16(32):86–96. - PubMed
-
- Centers for Disease Control and Prevention. National, state, and local area vaccination coverage among adolescents aged 13–17 years—United States, 2008. MMWR Morb Mortal Wkly Rep. 2009;58(36):997–1001. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

