Diastolic Cardiac Pathology and Clinical Twin-Twin Transfusion Syndrome in Monochorionic/Diamniotic Twins
- PMID: 21909155
- PMCID: PMC3169385
- DOI: 10.1016/j.ajog.2011.06.045
Diastolic Cardiac Pathology and Clinical Twin-Twin Transfusion Syndrome in Monochorionic/Diamniotic Twins
Abstract
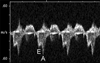
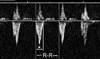
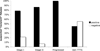
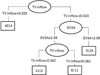
OBJECTIVE: to identify differences in echocardiographic profiles of monochorionic/diamniotic pregnancies with early or mild twin-twin transfusion syndrome (TTTS), compared to monochorionic/diamniotic twins affected only by discordant growth or discordant fluid. STUDY DESIGN: retrospective evaluation of sonograms and echocardiograms of twin pregnancies referred for suspected TTTS. RESULTS: 112 monochorionic/diamniotic pairs were studied. 41 did not have/develop TTTS, 61 had Stage I/II TTTS. Ten developed TTTS after initially not meeting criteria. TTTS recipients had a higher rate of venous Doppler or tricuspid inflow abnormalities than purported "recipients" in non-TTTS pregnancies (86% vs. 37%, P<0.001). TTTS recipients had shorter tricuspid inflow duration/RR intervals than non-TTTS fetuses (32+/-6% versus 37+/-4%, P<0.001). Logistic regression and recursive partitioning identified shorter tricuspid inflow duration, longer isovolumic relaxation, and ductus venosus abnormality associated with TTTS. CONCLUSION: Diastolic pathology, specifically shorter tricuspid inflow duration, may be considered a hallmark of TTTS distinguishing these pregnancies from other monochorionic/diamniotic twin complications.
Conflict of interest statement
Figures







Similar articles
-
Fetal ventricular strain in uncomplicated and selective growth-restricted monochorionic diamniotic twin pregnancies and cardiovascular response in pre-twin-twin transfusion syndrome.Ultrasound Obstet Gynecol. 2020 Nov;56(5):694-704. doi: 10.1002/uog.21911. Ultrasound Obstet Gynecol. 2020. PMID: 31682302 Free PMC article.
-
Modelling the influence of amnionicity on the severity of twin-twin transfusion syndrome in monochorionic twin pregnancies.Phys Med Biol. 2004 Mar 21;49(6):N57-64. doi: 10.1088/0031-9155/49/6/n01. Phys Med Biol. 2004. PMID: 15104328
-
Renal artery Doppler studies in the assessment of monochorionic, diamniotic twin pregnancies with and without twin-twin transfusion syndrome.Am J Obstet Gynecol MFM. 2020 Aug;2(3):100167. doi: 10.1016/j.ajogmf.2020.100167. Epub 2020 Jul 1. Am J Obstet Gynecol MFM. 2020. PMID: 33345886
-
Outcome of twin-twin transfusion syndrome according to Quintero stage of disease: systematic review and meta-analysis.Ultrasound Obstet Gynecol. 2020 Dec;56(6):811-820. doi: 10.1002/uog.22054. Epub 2020 Nov 12. Ultrasound Obstet Gynecol. 2020. PMID: 32330342
-
Monochorionic diamniotic twin pregnancies pregnancy outcome, risk stratification and lessons learnt from placental examination.Verh K Acad Geneeskd Belg. 2010;72(1-2):5-15. Verh K Acad Geneeskd Belg. 2010. PMID: 20726437 Review.
Cited by
-
Overview and Long-term Outcomes of Patients Born With Twin-to-Twin Transfusion Syndrome.Rev Obstet Gynecol. 2013;6(3-4):149-54. Rev Obstet Gynecol. 2013. PMID: 24826204 Free PMC article.
-
Assessment of fetal cardiac function in early fetal life: feasibility, reproducibility, and early fetal nomograms.AJOG Glob Rep. 2024 Feb 23;4(1):100325. doi: 10.1016/j.xagr.2024.100325. eCollection 2024 Feb. AJOG Glob Rep. 2024. PMID: 38586615 Free PMC article.
-
Fetal cardiovascular alterations in twin-to-twin transfusion syndrome.Med Pharm Rep. 2020 Jan;93(1):5-11. doi: 10.15386/mpr-1481. Epub 2020 Jan 31. Med Pharm Rep. 2020. PMID: 32133441 Free PMC article. Review.
-
Sensitive detection of hemodynamic changes after fetoscopic laser photocoagulation by assessing intraventricular pressure difference in fetuses with twin-to-twin transfusion syndrome.J Perinat Med. 2024 Aug 9;52(8):843-851. doi: 10.1515/jpm-2024-0147. Print 2024 Oct 28. J Perinat Med. 2024. PMID: 39118408
-
Evaluation and Management of Fetal Cardiac Function and Heart Failure.Curr Treat Options Cardiovasc Med. 2016 Sep;18(9):55. doi: 10.1007/s11936-016-0477-3. Curr Treat Options Cardiovasc Med. 2016. PMID: 27423668 Review.
References
-
- Urig MA, Clewell WH, Elliott JP. Twin-twin transfusion syndrome. Am J Obstet Gynecol. 1990;163:1522–1526. - PubMed
-
- Umur A, van Gemert MJ, Nikkels PG, Ross MG. Monochorionic twins and twin-twin transfusion syndrome: the protective role of arterio-arterial anastomoses. Placenta. 2002;23:201–209. - PubMed
-
- Machin GA, Bamforth F. Zygosity and placental anatomy in 15 consecutive sets of spontaneously conceived triplets. Am J Med Genet. 1996;61:247–252. - PubMed
-
- Hecher K, Plath H, Bregenzer T, Hansmann M, Hackeloer BJ. Endoscopic laser surgery versus serial amniocenteses in the treatment of severe twin-twin transfusion syndrome. Am J Obstet Gynecol. 1999;180:717–724. - PubMed
-
- Duncan KR, Denbow ML, Fisk NM. The aetiology and management of twin-twin transfusion syndrome. Prenat Diagn. 1997;17:1227–1236. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
