Diagnosis and treatment of neurocysticercosis
- PMID: 21912406
- PMCID: PMC3350327
- DOI: 10.1038/nrneurol.2011.135
Diagnosis and treatment of neurocysticercosis
Abstract
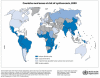
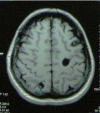
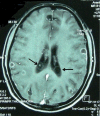
Neurocysticercosis is a parasitic disease caused by the larval (cystic) form of the pork cestode tapeworm, Taenia solium, and is a major cause of acquired seizures and epilepsy worldwide. Development of sensitive and specific diagnostic methods, particularly CT and MRI, has revolutionized our knowledge of the burden of cysticercosis infection and disease, and has led to the development of effective antihelminthic treatments for neurocysticercosis. The importance of calcified granulomas with perilesional edema as foci of seizures and epilepsy in populations where neurocysticercosis is endemic is newly recognized, and indicates that treatment with anti-inflammatory agents could have a role in controlling or preventing epilepsy in these patients. Importantly, neurocysticercosis is one of the few diseases that could potentially be controlled or eliminated-an accomplishment that would prevent millions of cases of epilepsy. This Review examines the rationale for treatment of neurocysticercosis and highlights the essential role of inflammation in the pathogenesis of disease, the exacerbation of symptoms that occurs as a result of antihelminthic treatment, and the limitations of current antihelminthic and anti-inflammatory treatments.
Figures






References
-
- Commission on Tropical Diseases of the International League Against Epilepsy Relationship between epilepsy and tropical diseases. Commission on Tropical Diseases of the International League Against Epilepsy. Epilepsia. 1994;35:89–93. - PubMed
-
- Garcia HH, Del Brutto OH. Neurocysticercosis: updated concepts about an old disease. Lancet Neurol. 2005;4:653–661. - PubMed
-
- Montano SM, Villaran MV, Ylquimiche L, Figueroa JJ, Rodriguez S, Bautista CT, Gonzalez AE, Tsang VC, Gilman RH, Garcia HH. Neurocysticercosis: association between seizures, serology, and brain CT in rural Peru. Neurology. 2005;65:229–233. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

