The use of magnetic resonance imaging to predict ACL graft structural properties
- PMID: 21962290
- PMCID: PMC3208804
- DOI: 10.1016/j.jbiomech.2011.09.004
The use of magnetic resonance imaging to predict ACL graft structural properties
Abstract
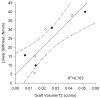
Magnetic resonance imaging (MRI) could potentially be used to non-invasively predict the strength of an ACL graft after ACL reconstruction. We hypothesized that the volume and T2 relaxation parameters of the ACL graft measured with MRI will predict the graft structural properties and anteroposterior (AP) laxity of the reconstructed knee. Nine goats underwent ACL reconstruction using a patellar tendon autograft augmented with a collagen or collagen-platelet composite. After 6 weeks of healing, the animals were euthanized, and the reconstructed knees were retrieved and imaged on a 3T scanner. AP laxity was measured prior to dissecting out the femur-graft-tibia constructs which were then tested to tensile failure to determine the structural properties. Regression analysis indicated a statistically significant relationship between the graft volume and the failure load (r(2)=0.502; p=0.049). When graft volume was normalized to the T2 relaxation time, the relationship was even greater (r(2)=0.687; p=0.011). There was a significant correlation between the graft volume and the linear stiffness (r(2)=0.847; p<0.001), which remained significant with T2 normalization (r(2)=0.764; p=0.002). For AP laxity at 30° flexion, there was not a significant correlation with graft volume, but there was a significant correlation with volume normalized by the T2 relaxation time (r(2)=0.512; p=0.046). These results suggest that MRI volumetric measures combined with graft T2 properties may be useful in predicting the structural properties of ACL grafts.
Copyright © 2011 Elsevier Ltd. All rights reserved.
Conflict of interest statement
Figures




References
-
- Anderson K, Seneviratne AM, Izawa K, Atkinson BL, Potter HG, Rodeo SA. Augmentation of tendon healing in an intraarticular bone tunnel with use of a bone growth factor. Am J Sports Med. 2001;29:689–698. - PubMed
-
- Arai Y, Hara K, Takahashi T, Urade H, Minami G, Takamiya H, Kubo T. Evaluation of the vascular status of autogenous hamstring tendon grafts after anterior cruciate ligament reconstruction in humans using magnetic resonance angiography. Knee Surg Sports Traumatol Arthrosc. 2008;16:342–347. - PubMed
-
- Fleming BC, Abate JA, Peura GD, Beynnon BD. The relationship between graft tensioning and the anterior-posterior laxity in the anterior cruciate ligament reconstructed goat knee. J Orthop Res. 2001;19:841–844. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

