In vitro and in vivo mechanical stability of orthodontic mini-implants
- PMID: 22011094
- PMCID: PMC8845555
- DOI: 10.2319/071311-447.1
In vitro and in vivo mechanical stability of orthodontic mini-implants
Abstract
Objective: To compare in vivo and in vitro mechanical stability of orthodontic mini-implants (OMIs) treated with a sandblasted, large-grit, and anodic-oxidation (SLAO) method vs those treated with a sandblasted, large-grit, and acid-etching (SLA) method.
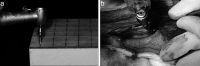
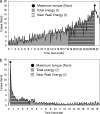
Materials and methods: Fifty-four titanium OMIs (cylindrical shape, drill-free type; diameter = 1.45 mm, length = 8 mm, Biomaterials Korea Inc, Seoul, Korea) were allocated into control, SLA, and SLAO groups (N = 12 for in vivo and N = 6 for in vitro studies per group). In vitro study was carried out on a polyurethane foam bone block (Sawbones, Pacific Research Laboratories Inc, Vashon, Wash). In vivo study was performed in the tibias of Beagles (6 males, age = 1 year, weight = 10 to 13 kg; OMIs were removed at 8 weeks after installation). For insertion and removal of OMIs, the speed and maximum torque of the surgical engine were set to 30 rpm and 40 Ncm, respectively. Maximum torque (MT), total energy (TE), and near peak energy (NPE) during the insertion and removal procedures were statistically analyzed.
Results: In the in vitro study, although the control group had a higher insertion MT value than the SLA and SLAO groups (P < .01), no differences in insertion TE and NPE or in any of the removal variables were noted among the three groups. In the in vivo study, the control group exhibited higher values for all insertion variables compared with the SLA and SLAO groups (MT, P < .001; TE, P < .01; NPE, P < .001). Although no difference in removal TE and removal NPE was noted among the three groups, the SLAO group presented with a higher removal MT than the SLA and control groups (P < .001).
Conclusions: SLAO treatment may be an effective tool in reducing insertion damage to surrounding tissue and improving the mechanical stability of OMIs.
Figures


References
-
- Miyawaki S, Koyama I, Inoue M, et al. Factors associated with the stability of titanium screws placed in the posterior region for orthodontic anchorage. Am J Orthod Dentofacial Orthop. 2003;124:373–378. - PubMed
-
- Cheng S. J, Tseng I. Y, Lee J. J, Kok S. H. A prospective study of the risk factors associated with failure of mini-implants used for orthodontic anchorage. Int J Oral Maxillofac Implants. 2004;19:100–106. - PubMed
-
- Chen C. H, Chang C. S, Hsieh C. H, et al. The use of microimplants in orthodontic anchorage. J Oral Maxillofac Surg. 2006;64:1209–1213. - PubMed
-
- Park H. S, Jeong S. H, Kwon O. W. Factors affecting the clinical success of screw implants used as orthodontic anchorage. Am J Orthod Dentofacial Orthop. 2006;130:18–25. - PubMed
-
- Motoyoshi M, Hirabahashi M, Uemura M, Shimizu N. Recommended placement torque tightening an orthodontic mini-implant. Clin Oral Implants Res. 2006;17:109–114. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Miscellaneous

