Transfusion of human volunteers with older, stored red blood cells produces extravascular hemolysis and circulating non-transferrin-bound iron
- PMID: 22021369
- PMCID: PMC3242722
- DOI: 10.1182/blood-2011-08-371849
Transfusion of human volunteers with older, stored red blood cells produces extravascular hemolysis and circulating non-transferrin-bound iron
Abstract
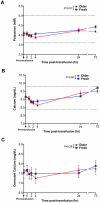
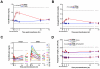
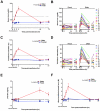
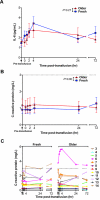
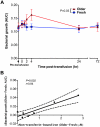
Transfusions of RBCs stored for longer durations are associated with adverse effects in hospitalized patients. We prospectively studied 14 healthy human volunteers who donated standard leuko-reduced, double RBC units. One unit was autologously transfused "fresh" (3-7 days of storage), and the other "older" unit was transfused after 40 to 42 days of storage. Of the routine laboratory parameters measured at defined times surrounding transfusion, significant differences between fresh and older transfusions were only observed in iron parameters and markers of extravascular hemolysis. Compared with fresh RBCs, mean serum total bilirubin increased by 0.55 mg/dL at 4 hours after transfusion of older RBCs (P = .0003), without significant changes in haptoglobin or lactate dehydrogenase. In addition, only after the older transfusion, transferrin saturation increased progressively over 4 hours to a mean of 64%, and non-transferrin-bound iron appeared, reaching a mean of 3.2μM. The increased concentrations of non-transferrin-bound iron correlated with enhanced proliferation in vitro of a pathogenic strain of Escherichia coli (r = 0.94, P = .002). Therefore, circulating non-transferrin-bound iron derived from rapid clearance of transfused, older stored RBCs may enhance transfusion-related complications, such as infection.
Trial registration: ClinicalTrials.gov NCT01319552.
Figures
References
-
- Ness PM. Does transfusion of stored red blood cells cause clinically important adverse effects? A critical question in search of an answer and a plan. Transfusion. 2011;51(4):666–667. - PubMed
-
- Koch CG, Li L, Sessler DI, et al. Duration of red-cell storage and complications after cardiac surgery. N Engl J Med. 2008;358(12):1229–1239. - PubMed
-
- Sanders J, Patel S, Cooper J, et al. Red blood cell storage is associated with length of stay and renal complications after cardiac surgery. Transfusion. 2011;51(11):2286–2294. - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

