Continuous controlled-infusion of hypertonic saline solution in traumatic brain-injured patients: a 9-year retrospective study
- PMID: 22035596
- PMCID: PMC3334811
- DOI: 10.1186/cc10522
Continuous controlled-infusion of hypertonic saline solution in traumatic brain-injured patients: a 9-year retrospective study
Abstract
Introduction: Description of a continuous hypertonic saline solution (HSS) infusion using a dose-adaptation of natremia in traumatic brain injured (TBI) patients with refractory intracranial hypertension (ICH).
Methods: We performed a single-center retrospective study in a surgical intensive care unit of a tertiary hospital. Fifty consecutive TBI patients with refractory ICH treated with continuous HSS infusion adapted to a target of natremia. In brief, a physician set a target of natremia adapted to the evolution of intracranial pressure (ICP). Flow of NaCl 20% was a priori calculated according to natriuresis, and the current and target natremia that were assessed every 4 hours.
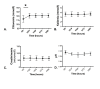
Results: The HSS infusion was initiated for a duration of 7 (5 to 10) (8 ± 4) days. ICP decreased from 29 (26 to 34) (31 ± 9) mm Hg at H0 to 20 (15 to 26) (21 ± 8) mm Hg at H1 (P < 0.05). Cerebral perfusion pressure increased from 61 (50 to 70) (61 ± 13) mm Hg at H0 up to 67 (60 to 79) (69 ± 12) mm Hg at H1 (P < 0.05). No rebound of ICH was reported after stopping continuous HSS infusion. Natremia increased from 140 (138 to 143) (140 ± 4) at H0 up to 144 (141 to 148) (144 ± 4) mmol/L at H4 (P < 0.05). Plasma osmolarity increased from 275 (268 to 281) (279 ± 17) mmol/L at H0 up to 290 (284 to 307) (297 ± 17) mmol/L at H24 (P < 0.05). The main side effect observed was an increase in chloremia from 111 (107 to 119) (113 ± 8) mmol/L at H0 up to 121 (117 to 124) (121 ± 6) mmol/L at H24 (P < 0.05). Neither acute kidney injury nor pontine myelinolysis was recorded.
Conclusions: Continuous HSS infusion adapted to close biologic monitoring enables long-lasting control of natremia in TBI patients along with a decreased ICP without any rebound on infusion discontinuation.
Figures



References
-
- Ke C, Poon WS, Ng HK, Lai FM, Tang NL, Pang JC. Impact of experimental acute hyponatremia on severe traumatic brain injury in rats: influences on injuries, permeability of blood-brain barrier, ultrastructural features, and aquaporin-4 expression. Exp Neurol. 2002;178:194–206. doi: 10.1006/exnr.2002.8037. - DOI - PubMed
-
- Brain Trauma Foundation; American Association of Neurological Surgeons; Congress of Neurological Surgeons. Guidelines for the management of severe traumatic brain injury. J Neurotrauma. 2007;24(Suppl 1):S1–106. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Molecular Biology Databases

