Reduction in hospital-wide mortality after implementation of a rapid response team: a long-term cohort study
- PMID: 22085785
- PMCID: PMC3388666
- DOI: 10.1186/cc10547
Reduction in hospital-wide mortality after implementation of a rapid response team: a long-term cohort study
Abstract
Introduction: Rapid response teams (RRTs) have been shown to reduce cardiopulmonary arrests outside the intensive care unit (ICU). Yet the utility of RRTs remains in question, as most large studies have failed to demonstrate a significant reduction in hospital-wide mortality after RRT implementation.
Methods: A cohort design with historical controls was used to determine the effect on hospital-wide mortality of an RRT in which clinical judgment, in addition to vital-signs criteria, was widely promoted as a key trigger for activation. All nonprisoner patients admitted to a tertiary referral public teaching hospital from 2003 through 2008 were included. In total, 77, 021 admissions before RRT implementation (2003 through 2005) and 79, 013 admissions after RRT implementation (2006 through 2008) were evaluated. The a priori primary outcome was unadjusted hospital-wide mortality. A Poisson regression model was then used to adjust for hospital-wide mortality trends over time. Secondary outcomes defined a priori were unadjusted out-of-ICU mortality and out-of-ICU cardiopulmonary-arrest codes.
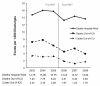
Results: In total, 855 inpatient RRTs (10.8 per 1, 000 hospital-wide discharges) were activated during the 3-year postintervention period. Forty-seven percent of RRTs were activated for reasons of clinical judgment. Hospital-wide mortality decreased from 15.50 to 13.74 deaths per 1, 000 discharges after RRT implementation (relative risk, 0.887; 95% confidence interval (CI), 0.817 to 0.963; P = 0.004). After adjusting for inpatient mortality trends over time, the reduction in hospital-wide mortality remained statistically significant (relative risk, 0.825; 95% CI, 0.694 to 0.981; P = 0.029). Out-of-ICU mortality decreased from 7.08 to 4.61 deaths per 1, 000 discharges (relative risk, 0.651; 95% CI, 0.570 to 0.743; P < 0.001). Out-of-ICU cardiopulmonary-arrest codes decreased from 3.28 to 1.62 codes per 1, 000 discharges (relative risk, 0.493; 95% CI, 0.399 to 0.610; P < 0.001).
Conclusions: Implementation of an RRT in which clinical judgment, in addition to vital-signs criteria, was widely cited as a rationale for activation, was associated with a significant reduction in hospital-wide mortality, out-of-ICU mortality, and out-of-ICU cardiopulmonary-arrest codes. The frequent use of clinical judgment as a criterion for RRT activation was associated with high RRT utilization.
Figures
References
-
- Zegers M, de Bruijne MC, Wagner C, Hoonhout LHF, Waaijman R, Smits M, Hout FAG, Zwaan L, Christiaans-Dingelhoff I, Timmermans DRM, Groenewegen PP, van der Wal G. Adverse events and potentially preventable deaths in Dutch hospitals: results of a retrospective patient record review study. Qual Saf Health Care. 2009;18:297–302. doi: 10.1136/qshc.2007.025924. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources

