The inflammasome promotes adverse cardiac remodeling following acute myocardial infarction in the mouse
- PMID: 22106299
- PMCID: PMC3241791
- DOI: 10.1073/pnas.1108586108
The inflammasome promotes adverse cardiac remodeling following acute myocardial infarction in the mouse
Abstract
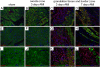
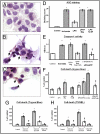
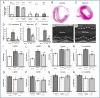
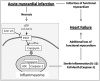
Acute myocardial infarction (AMI) initiates an intense inflammatory response that promotes cardiac dysfunction, cell death, and ventricular remodeling. The molecular events underlying this inflammatory response, however, are incompletely understood. In experimental models of sterile inflammation, ATP released from dying cells triggers, through activation of the purinergic P2X7 receptor, the formation of the inflammasome, a multiprotein complex necessary for caspase-1 activation and amplification of the inflammatory response. Here we describe the presence of the inflammasome in the heart in an experimental mouse model of AMI as evidenced by increased caspase-1 activity and cytoplasmic aggregates of the three components of the inflammasome--apoptosis speck-like protein containing a caspase-recruitment domain (ASC), cryopyrin, and caspase-1, localized to the granulation tissue and cardiomyocytes bordering the infarct. Cultured adult murine cardiomyocytes also showed the inducible formation of the inflammasome associated with increased cell death. P2X7 and cryopyrin inhibition (using silencing RNA or a pharmacologic inhibitor) prevented the formation of the inflammasome and limited infarct size and cardiac enlargement after AMI. The formation of the inflammasome in the mouse heart during AMI causes additional loss of functional myocardium, leading to heart failure. Modulation of the inflammasome may therefore represent a unique therapeutic strategy to limit cell death and prevent heart failure after AMI.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

References
-
- Rosamond W, et al. American Heart Association Statistics Committee and Stroke Statistics Subcommittee Heart disease and stroke statistics—2008 update: A report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation. 2008;117:e25–e146. - PubMed
-
- Greenberg H, McMaster P, Dwyer EM., Jr Left ventricular dysfunction after acute myocardial infarction: Results of a prospective multicenter study. J Am Coll Cardiol. 1984;4:867–874. - PubMed
-
- Goldberg RJ, et al. A 25-year perspective into the changing landscape of patients hospitalized with acute myocardial infarction (the Worcester Heart Attack Study) Am J Cardiol. 2004;94:1373–1378. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Molecular Biology Databases
Miscellaneous

