Cystic dystrophy of the duodenal wall is not always associated with chronic pancreatitis
- PMID: 22110260
- PMCID: PMC3218148
- DOI: 10.3748/wjg.v17.i39.4349
Cystic dystrophy of the duodenal wall is not always associated with chronic pancreatitis
Abstract
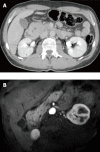
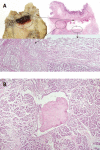
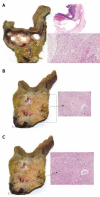
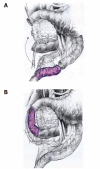
Cystic dystrophy of the duodenal wall is a rare form of the disease which was described in 1970 by French authors who reported the presence of focal pancreatic disease localized in an area comprising the C-loop of the duodenum and the head of the pancreas. German authors have defined this area as a "groove". We report our recent experience on cystic dystrophy of the paraduodenal space and systematically review the data in the literature regarding the alterations of this space. A MEDLINE search of papers published between 1966 and 2010 was carried out and 59 papers were considered for the present study; there were 19 cohort studies and 40 case reports. The majority of patients having groove pancreatitis were middle aged. Mean age was significantly higher in patients having groove carcinoma. The diagnosis of cystic dystrophy of the duodenal wall can now be assessed by multidetector computer tomography, magnetic resonance imaging and endoscopic ultrasonography. These latter two techniques may also add more information on the involvement of the remaining pancreatic gland not involved by the duodenal malformation and they may help in differentiating "groove pancreatitis" from "groove adenocarcinoma". In conclusion, chronic pancreatitis involving the entire pancreatic gland was present in half of the patients with cystic dystrophy of the duodenal wall and, in the majority of them, the pancreatitis had calcifications.
Keywords: Cystic dystrophy of duodenal wall; Outcome; Pancreatitis; Therapy.
Figures
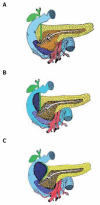
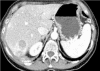
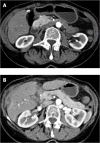
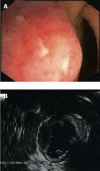
References
-
- Potet F, Duclert N. [Cystic dystrophy on aberrant pancreas of the duodenal wall] Arch Fr Mal App Dig. 1970;59:223–238. - PubMed
-
- Leger L, Lemaigre G, Lenriot JP. [Cysts on heterotopic pancreas of the duodenal wall] Nouv Presse Med. 1974;3:2309–2314. - PubMed
-
- Vankemmel M, Paris JC, Houcke M, Laurent JC, Burzynski A. [Paraduodenal cysts near Vater’s ampulla and chronic pancreatitis] Med Chir Dig. 1975;4:181–185. - PubMed
-
- Becker V, Mischke U. Groove pancreatitis. Int J Pancreatol. 1991;10:173–182. - PubMed
-
- Adsay NV, Zamboni G. Paraduodenal pancreatitis: a clinico-pathologically distinct entity unifying “cystic dystrophy of heterotopic pancreas”, “para-duodenal wall cyst”, and “groove pancreatitis”. Semin Diagn Pathol. 2004;21:247–254. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

