Fetoplacental vascular endothelial dysfunction as an early phenomenon in the programming of human adult diseases in subjects born from gestational diabetes mellitus or obesity in pregnancy
- PMID: 22144986
- PMCID: PMC3226353
- DOI: 10.1155/2011/349286
Fetoplacental vascular endothelial dysfunction as an early phenomenon in the programming of human adult diseases in subjects born from gestational diabetes mellitus or obesity in pregnancy
Abstract
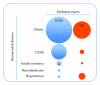
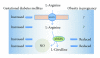
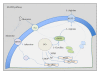
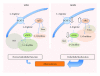
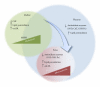
Gestational diabetes mellitus (GDM) and obesity in pregnancy (OP) are pathological conditions associated with placenta vascular dysfunction coursing with metabolic changes at the fetoplacental microvascular and macrovascular endothelium. These alterations are seen as abnormal expression and activity of the cationic amino acid transporters and endothelial nitric oxide synthase isoform, that is, the "endothelial L-arginine/nitric oxide signalling pathway." Several studies suggest that the endogenous nucleoside adenosine along with insulin, and potentially arginases, are factors involved in GDM-, but much less information regards their role in OP-associated placental vascular alterations. There is convincing evidence that GDM and OP prone placental endothelium to an "altered metabolic state" leading to fetal programming evidenced at birth, a phenomenon associated with future development of chronic diseases. In this paper it is suggested that this pathological state could be considered as a metabolic marker that could predict occurrence of diseases in adulthood, such as cardiovascular disease, obesity, diabetes mellitus (including gestational diabetes), and metabolic syndrome.
Copyright © 2011 Andrea Leiva et al.
Figures
References
-
- Sobrevia L, Casanello P. Placenta. In: Pérez-Sánchez A, Donoso-Siña E, editors. Obstetricia. Santiago, Chile: Mediterráneo; 2011. pp. 136–176.
-
- Casanello P, Escudero C, Sobrevia L. Equilibrative nucleoside (ENTs) and cationic amino acid (CATS) transporters: implications in foetal endothelial dysfunction in human pregnancy diseases. Current Vascular Pharmacology. 2007;5(1):69–84. - PubMed
-
- Ignarro LJ, Napoli C. Novel features of nitric oxide, endothelial nitric oxide synthase, and atherosclerosis. Current Diabetes Reports. 2005;5(1):17–23. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous
