Corticosteroids for treating hypotension in preterm infants
- PMID: 22161379
- PMCID: PMC7133776
- DOI: 10.1002/14651858.CD003662.pub4
Corticosteroids for treating hypotension in preterm infants
Abstract
Background: Systemic hypotension is a relatively common complication of preterm birth and is associated with periventricular haemorrhage, periventricular white matter injury and adverse neurodevelopmental outcome. Corticosteroid treatment has been used as an alternative or an adjunct to conventional treatment with volume expansion and vasopressor/inotropic therapy.
Objectives: To determine the effectiveness and safety of corticosteroids used either as primary treatment of hypotension or for the treatment of refractory hypotension in preterm infants.
Search methods: Randomized or quasi-randomised controlled trials were identified by searching the Cochrane Central Register of Controlled Trials (CENTRAL, The Cochrane Library, Issue 2, 2011), MEDLINE (1996 to Jan 2011), EMBASE (1974 to Jan 2011), CINAHL (1981 to 2011), reference lists of published papers and abstracts from the Pediatric Academic Societies and the European Society for Pediatric Research meetings published in Pediatric Research (1995 to 2011).
Selection criteria: We included all randomised or quasi-randomised controlled trials investigating the effect of corticosteroid therapy in the treatment of hypotension in preterm infants (< 37 weeks gestation) less than 28 days old. Studies using corticosteroids as primary treatment were included as well as studies using corticosteroids in babies with hypotension resistant to inotropes/pressors and volume therapy. We included studies comparing oral/intravenous corticosteroids with placebo, other drugs used for providing cardiovascular support or no therapy in this review.
Data collection and analysis: Methodological quality of eligible studies was assessed according to the methods used for minimising selection bias, performance bias, attrition bias and detection bias. Studies that evaluated corticosteroids (1) as primary treatment for hypotension or (2) for refractory hypotension unresponsive to prior use of inotropes/pressors and volume therapy, were analysed using separate comparisons. Data were analysed using the standard methods of the Neonatal Review Group using Rev Man 5.1.2. Treatment effect was analysed using relative risk, risk reduction, number needed to treat for categorical outcomes and weighted mean difference for outcomes measured on a continuous scale, with 95% confidence intervals.
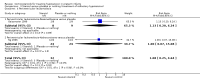
Main results: Four studies were included in this review enrolling a total of 123 babies. In one study, persistent hypotension was more common in hydrocortisone treated infants as compared to those who received dopamine as primary treatment for hypotension (RR 8.2, 95% CI 0.47 to 142.6; RD 0.19, 95% CI 0.01 to 0.37). In two studies comparing steroid versus placebo, persistent hypotension (defined as a continuing need for inotrope infusion) was less common in steroid treated infants as compared to controls who received placebo for refractory hypotension (RR 0.35, 95% CI 0.19 to 0.65; RD -0.47, 95% CI - 0.68 to - 0.26; NNT = 2.1, 95% CI 1.47, 3.8). There were no statistically significant effects on any other short or long-term outcome. A further two studies that have only been published in abstract form to date, may be eligible for inclusion in a future update of this review.
Authors' conclusions: Hydrocortisone may be as effective as dopamine when used as a primary treatment for hypotension. But the long term safety data on the use of hydrocortisone in this manner is unknown.Steroids are effective in treatment of refractory hypotension in preterm infants without an increase in short term adverse consequences. However, long term safety or benefit data is lacking. With long term benefit or safety data lacking steroids cannot be recommended routinely for the treatment of hypotension in preterm infants.
Conflict of interest statement
None known.
Figures



























Update of
-
Corticosteroids for treating hypotension in preterm infants.Cochrane Database Syst Rev. 2007 Jan 24;(1):CD003662. doi: 10.1002/14651858.CD003662.pub3. Cochrane Database Syst Rev. 2007. Update in: Cochrane Database Syst Rev. 2011 Dec 07;(12):CD003662. doi: 10.1002/14651858.CD003662.pub4. PMID: 17253493 Updated.
References
References to studies included in this review
Bourchier 1997 {published data only}
Gaissmaier 1999 {published data only}
-
- Gaissmaier RE, Pohlandt F. Single dose dexamethasone treatment of hypotension in preterm infants. Journal of Pediatrics 1999;134:701‐5. - PubMed
Hochwald 2010 {published and unpublished data}
-
- Hochwald O, Pelligra G, Osiovich H. The use of hydrocortisone for the treatment of hypotension in VLBW infants. Pediatric Academic Conference Proceedings. Available from http://www.abstracts2view.com/pasall/. 2010:Abstract 504.
Ng 2006 {published data only}
References to studies excluded from this review
Bonsante 2007 {published data only}
-
- Bonsante F, Latorre G, Iacobelli S, Forziati V, Laforgia N, Esposito L, et al. Early low‐dose hydrocortisone in very preterm infants: a randomized, placebo‐controlled trial. Neonatology 2007;91:217‐21. - PubMed
Efird 2005 {published data only}
-
- Efird MM, Heerens AT, Gordon PV, Bose CL, Young DA. A randomized controlled trial of prophylactic hydrocortisone supplementation for the prevention of hypotension in extremely low birth weight infants. Journal of Perinatology 2005;25:119‐24. - PubMed
Emery 1992 {published data only}
-
- Emery EF, Greenough A. Effect of dexamethasone on blood pressure ‐ Relationship to postnatal age. European Journal of Pediatrics 1992;151:364‐6. - PubMed
Fauser 1993 {published data only}
-
- Fauser A, Pohlandt F, Bartmann P, Gortner L. Rapid increase of blood pressure in extremely low birth weight infants after a single dose of dexamethasone. European Journal of Pediatrics 1993;152:354‐6. - PubMed
Fernandez 2005 {published data only}
-
- Fernandez E, Schrader R, Watterberg K. Prevalence of low cortisol values in term and near‐term infants with vasopressor‐resistant hypotension. Journal of Perinatology 2005;25:114‐8. - PubMed
Helbock 1993 {published data only}
-
- Helbock HJ, Insoft RM, Conte FA. Glucocorticoid‐responsive hypotension in extremely low birth weight newborns. Pediatrics 1993;92:715‐7. - PubMed
Juren 2003 {published data only}
-
- Juren T. The effect of the early hydrocortisone administration on the blood pressure in extremely low birth weight infants. Cesko‐Slovenska Pediatrie 2003;58:546‐51.
Kopelman 1999 {published data only}
-
- Kopelman AE, Moise AA, Holbert D, Hegemier SE. A single very early dexamethasone dose improves respiratory and cardiovascular adaptation in preterm infants. Journal of Pediatrics 1999;135:345‐50. - PubMed
Lespinasse 2001 {published data only}
-
- Lespinasse AA, Kamat M, Pildes R, Wilks A, Pyati S. Dexamethasone in critically ill term newborns with labile blood pressure. Pediatric Research 2001;49:268A.
Ng 2001 {published data only}
Ng 2004 {published data only}
-
- Ng PC, Fok TF, Liu F, Lee CH, Ma KC, Wong E. Effects of inhaled corticosteroids on systemic blood pressure in preterm infants. Biology of the Neonate 2004;86:201‐6. - PubMed
Noori 2002 {published data only}
-
- Noori S, Siassi B, Acherman RA, Sardesai SR, Ramanathan R. Cardiovascular responses to very low doses of dexamethasone in very low birth weight (VLBW) infants with refractory hypotension. Pediatric Research 2002;51:385A.
Noori 2006 {published data only}
-
- Noori S, Friedlich P, Wong P, Ebrahimi M, Siassi B, Seri I. Hemodynamic changes after low‐dosage hydrocortisone administration in vasopressor‐treated preterm and term neonates.. Pediatrics 2006;118:1456‐66. - PubMed
Ramanathan 1996 {published data only}
-
- Ramanathan R, Siassi B, Sardesai S, de‐Lamos R. Dexamethasone versus hydrocortisone for hypotension refractory to high dose inotropic agents and incidence of candida infection in extremely low birth weight infants. Pediatric Research 1996;39:240A.
Seri 2001 {published data only}
-
- Seri I, Tan R, Evans J. Cardiovascular effects of hydrocortisone in preterm infants with pressor‐resistant hypotension. Pediatrics 2001;107:1070‐4. - PubMed
Tantivit 1999 {published data only}
-
- Tantivit P, Subramanian N, Garg M, Ramanathan R, deLemos RA. Low serum cortisol in term newborns with refractory hypotension. Journal of Perinatology 1999;19:352‐7. - PubMed
Vanhole 2002 {published data only}
-
- Vanhole C, Naullers G, H Devilger, Berghe, Zegher F. Early low dose hydrocortisone treatment of preterm newborns. Pediatric Research 2002;52:783A.
Visveshwara 1996 {published data only}
-
- Visveshwara N, Peck M, Wells R, Bansal V, Chopra D, Rajani K. Efficacy of hydrocortisone in restoring blood pressure in infants on dopamine therapy. Pediatric Research 1996;39:251A.
References to studies awaiting assessment
Krediet 1998 {published data only}
-
- Krediet TG, Ent K, Rademaker KMA, Bel F. Rapid increase of blood pressure after low dose hydrocortisone (HC) in low birth weight neonates with hypotension refractory to high doses of cardio‐inotropics. Pediatric Research 1998;43:38A. [Abstract no. 210]
Osiovich 2000 {published data only}
-
- Osiovich H, Phillipos E, Lemke RP. A short course of hydrocortisone in hypotensive neonates < 1250 g in the first 24 hours of life: A randomized, double blind controlled trial. Pediatric Research 2000;47:422A. [Abstract no. 2498]
Additional references
Cunningham 1999
-
- Cunningham S, Symon AG, Elton RA, Zhu C, McIntosh N. Intra‐arterial blood pressure reference ranges, death and morbidity in very low birthweight infants during the first seven days of life. Early Human Development 1999;56:151‐65. - PubMed
Goldstein 1995
-
- Goldstein RF, Thompson RJ Jr, Oehler J M, Brazy JE. Influence of acidosis, hypoxaemia, and hypotension on neurodevelopmental outcome in very low birth weight infants. Pediatrics 1995;95:238‐43. - PubMed
Halliday 2010
Kluckow 1996
-
- Kluckow M, Evans N. Relationship between blood pressure and cardiac output in preterm infants requiring mechanical ventilation. Relationship between blood pressure and cardiac output in preterm infants requiring mechanical ventilation. Journal of Pediatrics 1996;129:506‐12. - PubMed
Kuint 2009
-
- Kuint J, Barak M, Morag I, Maayan‐Metzger A. Early treated hypotension and outcome in very low birth weight infants. Neonatology 2009;95:311‐6. [PUBMED: 19052477 ] - PubMed
Lee 1999
Martens 2003
-
- Martens SE, Rijken M, Stoelhorst GM, Zwieten PH, Zwinderman AH, Wit JM, et al. Is hypotension a major risk factor for neurological morbidity at term age in very preterm infants?. Early Human Development 2003;75:79‐89. [PUBMED: 14652161 ] - PubMed
Miall‐Allen 1987
Moise 1995
-
- Moise AA, Wearden ME, Kozinetz CA, Gest AL, Welty SE, Hansen TN. Antenatal steroids are associated with less need for blood pressure support in extremely premature infants. Pediatrics 1995;95:845‐50. - PubMed
Papile 1978
-
- Papile LA, Burstein J, Burstein R, Koffler H. PPapile LA, Burstein J, Burstein R, Koffler H. Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. Journal of Pediatrics 1978;92:529‐34. - PubMed
Pladys 1999
-
- Pladys P, Wodey E, Beuchee A, Branger B, Betremieux P. Left ventricle output and mean arterial blood pressure in preterm infants during the 1st day of life. European Journal of Pediatrics 1999;158:817‐24. - PubMed
Sasidharan 1998
-
- Sasidharan P. Role of corticosteroids in neonatal blood pressure homeostasis. Clinics in Perinatology 1998;25:723‐40, xi. Review. - PubMed
Scott 1995
-
- Scott SM, Watterberg KL. Effect of gestational age, postnatal age, and illness on plasma cortisol concentrations in premature infants. Pediatric Research 1995;37:112‐6. - PubMed
Watterberg 2002
-
- Watterberg KL. Adrenal insufficiency and cardiac dysfunction in the preterm infant. Pediatric Research 2002;51:422‐4. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

