Mid-term clinical results of minimally invasive decompression and posterolateral fusion with percutaneous pedicle screws versus conventional approach for degenerative spondylolisthesis with spinal stenosis
- PMID: 22173610
- PMCID: PMC3366131
- DOI: 10.1007/s00586-011-2114-x
Mid-term clinical results of minimally invasive decompression and posterolateral fusion with percutaneous pedicle screws versus conventional approach for degenerative spondylolisthesis with spinal stenosis
Abstract
Introduction: In order to minimize perioperative invasiveness and improve the patients' functional capacity of daily living, we have performed minimally invasive lumbar decompression and posterolateral fusion (MIS-PLF) with percutaneous pedicle screw fixation for degenerative spondylolisthesis with spinal stenosis. Although several minimally invasive fusion procedures have been reported, no study has yet demonstrated the efficacy of MIS-PLF in degenerative spondylolisthesis of the lumbar spine. This study prospectively compared the mid-term clinical outcome of MIS-PLF with those of conventional PLF (open-PLF) focusing on perioperative invasiveness and patients' functional capacity of daily living.
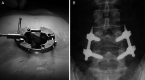
Materials and methods: A total of 80 patients received single-level PLF for lumbar degenerative spondylolisthesis with spinal stenosis. There were 43 cases of MIS-PLF and 37 cases of open-PLF. The surgical technique of MIS-PLF included making a main incision (4 cm), and neural decompression followed by percutaneous pedicle screwing and rod insertion. The posterolateral gutter including the medial transverse process was decorticated and iliac bone graft was performed. The parameters analyzed up to a 2-year period included the operation time, intra and postoperative blood loss, Oswestry-Disability Index (ODI), Roland-Morris Questionnaire (RMQ), the Japanese Orthopaedic Association score, and the visual analogue scale of low back pain. The fusion rate and complications were also reviewed.
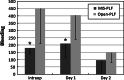
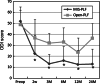
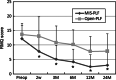
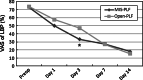
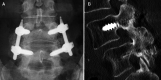
Results: The average operation time was statistically equivalent between the two groups. The intraoperative blood loss was significantly less in the MIS-PLF group (181 ml) when compared to the open-PLF group (453 ml). The postoperative bleeding on day 1 was also less in the MIS-PLF group (210 ml) when compared to the open-PLF group (406 ml). The ODI and RMQ scores rapidly decreased during the initial postoperative 2 weeks in the MIS-PLF group, and consistently maintained lower values than those in the open-PLF group at 3, 6, 12, and 24 months postoperatively. The fusion rate was statistically equivalent between the two groups (98 vs. 100%), and no major complications occurred.
Conclusion: The MIS-PLF utilizing a percutaneous pedicle screw system is less invasive compared to conventional open-PLF. The reduction in postoperative pain led to an increase in activity of daily living (ADL), demonstrating rapid improvement of several functional parameters. This superiority in the MIS-PLF group was maintained until 2 years postoperatively, suggesting that less invasive PLF offers better mid-term results in terms of reducing low back pain and improving patients' functional capacity of daily living. The MIS-PLF utilizing percutaneous pedicle screw fixation serves as an alternative technique, eliminating the need for conventional open approach.
Figures

Similar articles
-
[Two different techniques combined with MIS-TLIF in the treatment of degenerative lumbar spondylolisthesis:a case-control study].Zhongguo Gu Shang. 2022 May 25;35(5):409-17. doi: 10.12200/j.issn.1003-0034.2022.05.002. Zhongguo Gu Shang. 2022. PMID: 35535527 Chinese.
-
Good clinical outcomes and fusion rate of facet fusion with a percutaneous pedicle screw system for degenerative lumbar spondylolisthesis: minimally invasive evolution of posterolateral fusion.Spine (Phila Pa 1976). 2015 May 1;40(9):E552-7. doi: 10.1097/BRS.0000000000000842. Spine (Phila Pa 1976). 2015. PMID: 25705957
-
Percutaneous Endoscopic Robot-Assisted Transforaminal Lumbar Interbody Fusion (PE RA-TLIF) for Lumbar Spondylolisthesis: A Technical Note and Two Years Clinical Results.Pain Physician. 2022 Jan;25(1):E73-E86. Pain Physician. 2022. PMID: 35051154
-
Lumbar Spinal Stenosis Associated With Degenerative Lumbar Spondylolisthesis: A Systematic Review and Meta-analysis of Secondary Fusion Rates Following Open vs Minimally Invasive Decompression.Neurosurgery. 2017 Mar 1;80(3):355-367. doi: 10.1093/neuros/nyw091. Neurosurgery. 2017. PMID: 28362963
-
Posterolateral fusion (PLF) versus transforaminal lumbar interbody fusion (TLIF) for spondylolisthesis: a systematic review and meta-analysis.Spine J. 2018 Jun;18(6):1088-1098. doi: 10.1016/j.spinee.2018.01.028. Epub 2018 Feb 13. Spine J. 2018. PMID: 29452283
Cited by
-
Postoperative Evaluation of Health-Related Quality-of-Life (HRQoL) of Patients With Lumbar Degenerative Spondylolisthesis After Instrumented Posterolateral Fusion (PLF): A prospective Study With a 2-Year Follow-Up.Open Orthop J. 2017 Dec 11;11:1423-1431. doi: 10.2174/1874325001711011423. eCollection 2017. Open Orthop J. 2017. PMID: 29387287 Free PMC article.
-
A More Efficient and Safer Improved Percutaneous Pedicle Screw Insertion Technique-Trajectory Dynamic Adjustment Technique, Technical Note, and Clinical Efficacy.Orthop Surg. 2025 Jan;17(1):82-93. doi: 10.1111/os.14260. Epub 2024 Oct 15. Orthop Surg. 2025. PMID: 39406475 Free PMC article.
-
Comparison of patient-controlled epidural analgesia and patient-controlled intravenous analgesia after spinal fusion surgery: a meta-analysis of randomized controlled trials.BMC Musculoskelet Disord. 2015 Dec 15;16:388. doi: 10.1186/s12891-015-0849-y. BMC Musculoskelet Disord. 2015. PMID: 26671684 Free PMC article.
-
Finite element analysis of different pedicle screw internal fixations for first lumbar vertebral fracture in different sports conditions.J Int Med Res. 2024 Mar;52(3):3000605241236054. doi: 10.1177/03000605241236054. J Int Med Res. 2024. PMID: 38468383 Free PMC article.
-
Robotic-assisted spine surgery allows for increased pedicle screw sizes while still improving safety as indicated by elevated triggered electromyographic thresholds.J Robot Surg. 2023 Jun;17(3):1007-1012. doi: 10.1007/s11701-022-01493-8. Epub 2022 Nov 30. J Robot Surg. 2023. PMID: 36449203 Free PMC article.
References
-
- Foley KT, Holly LT, Schwender JD. Minimally invasive lumbar fusion. Spine. 2003;28:S26–S35. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

