Prevalence of metabolic syndrome and metabolic abnormalities in schizophrenia and related disorders--a systematic review and meta-analysis
- PMID: 22207632
- PMCID: PMC3576174
- DOI: 10.1093/schbul/sbr148
Prevalence of metabolic syndrome and metabolic abnormalities in schizophrenia and related disorders--a systematic review and meta-analysis
Abstract
Individuals with schizophrenia have high levels of medical comorbidity and cardiovascular risk factors. The presence of 3 or more specific factors is indicative of metabolic syndrome, which is a significant influence upon future morbidity and mortality. We aimed to clarify the prevalence and predictors of metabolic syndrome (MetS) in adults with schizophrenia and related disorders, accounting for subgroup differences. A PRISMA systematic search, appraisal, and meta-analysis were conducted of 126 analyses in 77 publications (n = 25,692). The overall rate of MetS was 32.5% (95% CI = 30.1%-35.0%), and there were only minor differences according to the different definitions of MetS, treatment setting (inpatient vs outpatient), by country of origin and no appreciable difference between males and females. Older age had a modest influence on the rate of MetS (adjusted R(2) = .20; P < .0001), but the strongest influence was of illness duration (adjusted R(2) = .35; P < .0001). At a study level, waist size was most useful in predicting high rate of MetS with a sensitivity of 79.4% and a specificity of 78.8%. Sensitivity and specificity of high blood pressure, high triglycerides, high glucose and low high-density lipoprotein, and age (>38 y) are shown in supplementary appendix 2 online. Regarding prescribed antipsychotic medication, highest rates were seen in those prescribed clozapine (51.9%) and lowest rates of MetS in those who were unmedicated (20.2%). Present findings strongly support the notion that patients with schizophrenia should be considered a high-risk group. Patients with schizophrenia should receive regular monitoring and adequate treatment of cardio-metabolic risk factors.
Figures
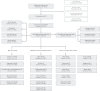







References
-
- Mitchell AJ, Malone D. Physical health and schizophrenia. Curr Opin Psychiatry. 2006;19:432–437. - PubMed
-
- Fleischhacker WW, Cetkovich-Bakmas M, De Hert M, et al. Comorbid somatic illnesses in patients with severe mental disorders: clinical, policy, and research challenges. J Clin Psychiatry. 2007;69:514–519. - PubMed
-
- Leucht S, Burkard T, Henderson J, et al. Physical illness and schizophrenia: a review of the literature. Acta Psychiatr Scand. 2007;116:317–333. - PubMed
-
- De Hert M, Dekker JM, Wood D, et al. Cardiovascular disease and diabetes in people with severe mental illness position statement from the European Psychiatric Association (EPA), supported by the European Association for the Study of Diabetes (EASD) and the European Society of Cardiology (ESC) Eur Psychiatry. 2009;24:412–424. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

