Prevalence and prognostic value of left ventricular diastolic dysfunction in idiopathic and heritable pulmonary arterial hypertension
- PMID: 22207680
- PMCID: PMC3367485
- DOI: 10.1378/chest.11-1903
Prevalence and prognostic value of left ventricular diastolic dysfunction in idiopathic and heritable pulmonary arterial hypertension
Abstract
Background: Little is known about the association between left ventricular (LV) diastolic dysfunction and outcomes in patients with idiopathic or heritable pulmonary arterial hypertension (PAH). Our rationale was to investigate the prevalence of LV diastolic dysfunction, and its association with disease severity and outcomes, in patients with idiopathic or heritable PAH.
Methods: Using the Cleveland Clinic Pulmonary Hypertension Registry, we identified subjects with heritable or idiopathic PAH who underwent Doppler echocardiography and right-sided heart catheterization. Echocardiographic diastolic parameters were assessed in each patient.
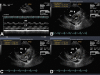
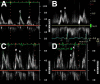
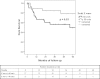
Results: A total of 61 patients met the inclusion criteria (idiopathic 85%, heritable 15%). The age at the time of echocardiography was 48.3 ± 18 years, 84% of the subjects were women, and 48% were on PAH-targeted therapies. Normal LV diastolic function, impaired relaxation, and pseudonormalization were seen in 10%, 88%, and 2% of the patients, respectively. Peak early diastolic (peak E) velocity was directly associated with LV end-diastolic volume and cardiac index and inversely associated with the degree of right ventricular dilation, right atrial pressure, and pulmonary vascular resistance. Peak E velocity was associated with mortality adjusted for age and sex (hazard ratio [HR], 1.5; 95% CI, 1.1-2 per 10 cm/s decrease; P = .015) and age, sex, 6-min walk distance, and cardiac output (HR, 1.8; 95% CI, 1.2-2.9 per 10 cm/s decrease; P = .01).
Conclusions: LV diastolic dysfunction of the impaired relaxation type is observed in the majority of patients with advanced idiopathic or heritable PAH. A decrease in transmitral flow peak E velocity is associated with worse hemodynamics and outcome.
Figures
Comment in
-
Diastolic dysfunction with nondilated left atrium.Chest. 2013 Jan;143(1):272-273. doi: 10.1378/chest.12-2032. Chest. 2013. PMID: 23276858 No abstract available.
-
Response.Chest. 2013 Jan;143(1):273-274. doi: 10.1378/chest.12-2145. Chest. 2013. PMID: 23276860 Free PMC article. No abstract available.
Similar articles
-
Impaired left ventricular mechanics in pulmonary arterial hypertension: identification of a cohort at high risk.Circ Heart Fail. 2013 Jul;6(4):748-55. doi: 10.1161/CIRCHEARTFAILURE.112.000098. Epub 2013 May 24. Circ Heart Fail. 2013. PMID: 23709658
-
Impact of Pulmonary Hemodynamics and Ventricular Interdependence on Left Ventricular Diastolic Function in Children With Pulmonary Hypertension.Circ Cardiovasc Imaging. 2016 Sep;9(9):10.1161/CIRCIMAGING.116.004612 e004612. doi: 10.1161/CIRCIMAGING.116.004612. Circ Cardiovasc Imaging. 2016. PMID: 27581953 Free PMC article.
-
[Relationship between systolic and diastolic function of the left ventricle in patients with impaired relaxation of the left ventricle without symptoms of heart failure. Attempt at quantitative estimation of diastolic function in the impaired relaxation stage].Pol Arch Med Wewn. 1997 Nov;98(11):414-23. Pol Arch Med Wewn. 1997. PMID: 9594559 Clinical Trial. Polish.
-
Clinical aspects of left ventricular diastolic function assessed by Doppler echocardiography following acute myocardial infarction.Dan Med Bull. 2001 Nov;48(4):199-210. Dan Med Bull. 2001. PMID: 11767125 Review.
-
[Evaluation of left ventricular diastolic function using Doppler echocardiography].Med Pregl. 1999 Jan-Feb;52(1-2):13-8. Med Pregl. 1999. PMID: 10352498 Review. Croatian.
Cited by
-
The heart in congenital diaphragmatic hernia: Knowns, unknowns, and future priorities.Front Pediatr. 2022 Aug 16;10:890422. doi: 10.3389/fped.2022.890422. eCollection 2022. Front Pediatr. 2022. PMID: 36052357 Free PMC article. Review.
-
Assessing the optimal MAP target in pre-capillary PH patients with RV failure: A retrospective analysis.Pulm Circ. 2023 Oct 8;13(4):e12292. doi: 10.1002/pul2.12292. eCollection 2023 Oct. Pulm Circ. 2023. PMID: 37817916 Free PMC article.
-
Diastolic Dysfunction Increases the Risk of Primary Graft Dysfunction after Lung Transplant.Am J Respir Crit Care Med. 2016 Jun 15;193(12):1392-400. doi: 10.1164/rccm.201508-1522OC. Am J Respir Crit Care Med. 2016. PMID: 26745666 Free PMC article.
-
Impact of Pre-Transplant Left Ventricular Diastolic Pressure on Primary Graft Dysfunction after Lung Transplantation: A Narrative Review.Diagnostics (Basel). 2024 Jun 24;14(13):1340. doi: 10.3390/diagnostics14131340. Diagnostics (Basel). 2024. PMID: 39001230 Free PMC article. Review.
-
Pulmonary hypertension in patients with heart failure and preserved ejection fraction: differential diagnosis and management.Pulm Circ. 2016 Mar;6(1):3-14. doi: 10.1086/685021. Pulm Circ. 2016. PMID: 27162611 Free PMC article. Review.
References
-
- Moustapha A, Kaushik V, Diaz S, Kang SH, Barasch E. Echocardiographic evaluation of left-ventricular diastolic function in patients with chronic pulmonary hypertension. Cardiology. 2001;95(2):96–100. - PubMed
-
- Ruan Q, Nagueh SF. Clinical application of tissue Doppler imaging in patients with idiopathic pulmonary hypertension. Chest. 2007;131(2):395–401. - PubMed
-
- Gurudevan SV, Malouf PJ, Auger WR, et al. Abnormal left ventricular diastolic filling in chronic thromboembolic pulmonary hypertension: true diastolic dysfunction or left ventricular underfilling? J Am Coll Cardiol. 2007;49(12):1334–1339. - PubMed
-
- Marcus JT, Vonk Noordegraaf A, Roeleveld RJ, et al. Impaired left ventricular filling due to right ventricular pressure overload in primary pulmonary hypertension: noninvasive monitoring using MRI. Chest. 2001;119(6):1761–1765. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

