Hyperinsulinemia enhances c-Myc-mediated mammary tumor development and advances metastatic progression to the lung in a mouse model of type 2 diabetes
- PMID: 22226054
- PMCID: PMC3496123
- DOI: 10.1186/bcr3089
Hyperinsulinemia enhances c-Myc-mediated mammary tumor development and advances metastatic progression to the lung in a mouse model of type 2 diabetes
Abstract
Introduction: Hyperinsulinemia, which is common in early type 2 diabetes (T2D) as a result of the chronically insulin-resistant state, has now been identified as a specific factor which can worsen breast cancer prognosis. In breast cancer, a high rate of mortality persists due to the emergence of pulmonary metastases.
Methods: Using a hyperinsulinemic mouse model (MKR+/+) and the metastatic, c-Myc-transformed mammary carcinoma cell line Mvt1, we investigated how high systemic insulin levels would affect the progression of orthotopically inoculated primary mammary tumors to lung metastases.
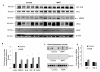
Results: We found that orthotopically injected Mvt1 cells gave rise to larger mammary tumors and to a significantly higher mean number of pulmonary macrometastases in hyperinsulinemic mice over a period of six weeks (hyperinsulinemic, 19.4 ± 2.7 vs. control, 4.0 ± 1.3). When Mvt1-mediated mammary tumors were allowed to develop and metastasize for approximately two weeks and were then surgically removed, hyperinsulinemic mice demonstrated a significantly higher number of lung metastases after a four-week period (hyperinsulinemic, 25.1 ± 4.6 vs. control, 7.4 ± 0.42). Similarly, when Mvt1 cells were injected intravenously, hyperinsulinemic mice demonstrated a significantly higher metastatic burden in the lung than controls after a three-week period (hyperinsulinemic, 6.0 ± 1.63 vs. control, 1.5 ± 0.68). Analysis of Mvt1 cells both in vitro and in vivo revealed a significant up-regulation of the transcription factor c-Myc under hyperinsulinemic conditions, suggesting that hyperinsulinemia may promote c-Myc signaling in breast cancer. Furthermore, insulin-lowering therapy using the beta-adrenergic receptor agonist CL-316243 reduced metastatic burden in hyperinsulinemic mice to control levels.
Conclusions: Hyperinsulinemia in a mouse model promotes breast cancer metastasis to the lung. Therapies to reduce insulin levels in hyperinsulinemic patients suffering from breast cancer could lessen the likelihood of metastatic progression.
Figures




Similar articles
-
Insulin-sensitizing therapy attenuates type 2 diabetes-mediated mammary tumor progression.Diabetes. 2010 Mar;59(3):686-93. doi: 10.2337/db09-1291. Epub 2009 Dec 3. Diabetes. 2010. PMID: 19959755 Free PMC article.
-
Insulin-mediated acceleration of breast cancer development and progression in a nonobese model of type 2 diabetes.Cancer Res. 2010 Jan 15;70(2):741-51. doi: 10.1158/0008-5472.CAN-09-2141. Epub 2010 Jan 12. Cancer Res. 2010. PMID: 20068149 Free PMC article.
-
Hyperinsulinemia promotes metastasis to the lung in a mouse model of Her2-mediated breast cancer.Endocr Relat Cancer. 2013 May 21;20(3):391-401. doi: 10.1530/ERC-12-0333. Print 2013 Jun. Endocr Relat Cancer. 2013. PMID: 23572162 Free PMC article.
-
EMT reversal in human cancer cells after IR knockdown in hyperinsulinemic mice.Endocr Relat Cancer. 2016 Sep;23(9):747-58. doi: 10.1530/ERC-16-0142. Epub 2016 Jul 19. Endocr Relat Cancer. 2016. PMID: 27435064 Free PMC article.
-
Insulin Resistance: The Increased Risk of Cancers.Curr Oncol. 2024 Feb 13;31(2):998-1027. doi: 10.3390/curroncol31020075. Curr Oncol. 2024. PMID: 38392069 Free PMC article. Review.
Cited by
-
Silencing vimentin expression decreases pulmonary metastases in a pre-diabetic mouse model of mammary tumor progression.Oncogene. 2017 Mar;36(10):1394-1403. doi: 10.1038/onc.2016.305. Epub 2016 Aug 29. Oncogene. 2017. PMID: 27568979 Free PMC article.
-
Childhood Obesity: A Potential Key Factor in the Development of Glioblastoma Multiforme.Life (Basel). 2022 Oct 21;12(10):1673. doi: 10.3390/life12101673. Life (Basel). 2022. PMID: 36295107 Free PMC article. Review.
-
The insulin and IGF signaling pathway sustains breast cancer stem cells by IRS2/PI3K-mediated regulation of MYC.Cell Rep. 2022 Dec 6;41(10):111759. doi: 10.1016/j.celrep.2022.111759. Cell Rep. 2022. PMID: 36476848 Free PMC article.
-
Hyperinsulinemia promotes aberrant histone acetylation in triple-negative breast cancer.Epigenetics Chromatin. 2019 Jul 17;12(1):44. doi: 10.1186/s13072-019-0290-9. Epigenetics Chromatin. 2019. PMID: 31315653 Free PMC article.
-
Insulin receptor phosphorylation by endogenous insulin or the insulin analog AspB10 promotes mammary tumor growth independent of the IGF-I receptor.Diabetes. 2013 Oct;62(10):3553-60. doi: 10.2337/db13-0249. Epub 2013 Jul 8. Diabetes. 2013. PMID: 23835331 Free PMC article.
References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

