Critical appraisal of ticagrelor in the management of acute coronary syndrome
- PMID: 22241944
- PMCID: PMC3253754
- DOI: 10.2147/TCRM.S19835
Critical appraisal of ticagrelor in the management of acute coronary syndrome
Abstract
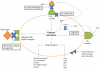
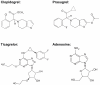
Ticagrelor is a novel P2Y₁₂ receptor antagonist which, like clopidogrel and prasugrel, functions by blocking adenosine diphosphate-mediated platelet aggregation. However, unlike the aforementioned agents, the binding of ticagrelor to this receptor is reversible. Ticagrelor is also believed to mediate some of its beneficial effects by augmenting the effects of adenosine, which is another unique pharmacologic property of this drug. In terms of antiplatelet effect, ticagrelor is more potent than clopidogrel and produces a faster and stronger inhibition of platelet aggregation. This may also be an advantage of ticagrelor over prasugrel, but this has not been adequately studied. Due to the reversible nature of the binding of ticagrelor to the platelet receptor, ticagrelor has a relatively fast offset of effect, with platelet aggregation approaching pretreatment levels about 3 days after discontinuation of therapy. This has advantages in patients requiring invasive procedures, but also makes medication adherence very important in order to be able to maintain an effective antiplatelet effect. Ticagrelor has been shown to be clinically superior to clopidogrel when given to patients with an acute coronary syndrome, resulting in significantly lower rates of myocardial infarction and vascular death. However, ticagrelor is indicated to be administered with aspirin, and the clinical benefits of ticagrelor may be less when daily dosages of aspirin exceed 100 mg. As expected, bleeding is the most common adverse effect with ticagrelor, although it occurs at rates comparable with those seen for clopidogrel with the exception of noncoronary artery bypass graft-related major bleeding and fatal intracranial bleeds, the latter of which occurs only rarely. Dyspnea is another common adverse effect with ticagrelor, although this is usually not severe and resolves with drug discontinuation. Unlike clopidogrel, there are no known pharmacogenomic concerns with ticagrelor, and emerging data suggest ticagrelor to be effective in patients resistant to clopidogrel, although more study is needed on this topic. While preliminary data suggest ticagrelor to be cost effective when compared with generic clopidogrel, the acquisition cost of ticagrelor is not insignificant and this will likely be an issue for many health care organizations. Currently, ticagrelor is well positioned to assume an active role in the treatment of coronary artery disease due to an impressive efficacy profile and reasonable safety. Its ultimate role in therapy will continue to evolve as studies on this drug continue eg, (Prevention of Cardiovascular Events in Patients with Prior Heart Attack Using Ticagrelor Compared to Placebo on a Background of Aspirin, PEGASUS) and more information hopefully becomes available on its use in clopidogrel nonresponders and relative safety and efficacy compared with prasugrel.
Keywords: P2Y12; adenosine receptor antagonist; ticagrelor.
Figures

References
-
- Dib C, Hanna E, Abu-Fadel M. A new era for antiplatelet therapy in patients with acute coronary syndrome. Am J Med Sci. 2010;340:407–411. - PubMed
-
- Kushner FG, Hand M, Smith SC, et al. 2009 focused updates: ACC/ AHA Guidelines for the Management of Patients With ST-Elevation Myocardial Infarction. J Am Coll Cardiol. 2009;54:2205–2241. - PubMed
-
- Wright RS, Anderson JL, Adams CD, et al. ACCF/AHA focused update of the guidelines for the management of patients with unstable angina/non ST-elevation myocardial infarction. J Am Coll Cardiol. 2011;2011;57:1920–1959. - PubMed
LinkOut - more resources
Full Text Sources
Molecular Biology Databases
Research Materials

