Protective effect of delayed remote limb ischemic postconditioning: role of mitochondrial K(ATP) channels in a rat model of focal cerebral ischemic reperfusion injury
- PMID: 22274742
- PMCID: PMC3345910
- DOI: 10.1038/jcbfm.2011.199
Protective effect of delayed remote limb ischemic postconditioning: role of mitochondrial K(ATP) channels in a rat model of focal cerebral ischemic reperfusion injury
Abstract
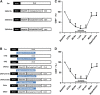
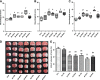
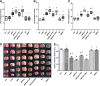
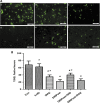
Delayed remote ischemic postconditioning (DRIPost) has been shown to protect the rat brain from ischemic injury. However, extremely short therapeutic time windows hinder its translational use and the mechanism of action remains elusive. Because opening of the mitochondria K(ATP) channel is crucial for cell apoptosis, we hypothesized that the neuroprotective effect of DRIPost may be associated with K(ATP) channels. In the present study, the neuroprotective effects of DRIPost were investigated using adult male Sprague-Dawley rats. Rats were exposed to 90 minutes of middle cerebral artery occlusion followed by 72 hours of reperfusion. Delayed remote ischemic postconditioning was performed with three cycles of bilateral femoral artery occlusion/reperfusion for 5 minutes at 3 or 6 hours after reperfusion. Neurologic deficit scores and infarct volumes were assessed, and cellular apoptosis was monitored by terminal deoxynucleotidyl transferase nick-end labeling. Our results showed that DRIPost applied at 6 hours after reperfusion exerted neuroprotective effects. The K(ATP) opener, diazoxide, protected rat brains from ischemic injury, while the K(ATP) blocker, 5-hydroxydecanote, reversed the neuroprotective effects of DRIPost. These findings indicate that DRIPost reduces focal cerebral ischemic injury and that the neuroprotective effects of DRIPost may be achieved through opening of K(ATP) channels.
Figures
Similar articles
-
Noninvasive delayed limb ischemic preconditioning attenuates myocardial ischemia-reperfusion injury in rats by a mitochondrial K(ATP) channel-dependent mechanism.Physiol Res. 2011;60(2):271-9. doi: 10.33549/physiolres.931944. Epub 2010 Nov 29. Physiol Res. 2011. PMID: 21114361
-
Morphine postconditioning protects against reperfusion injury in the isolated rat hearts.J Surg Res. 2008 Apr;145(2):287-94. doi: 10.1016/j.jss.2007.07.020. Epub 2007 Aug 23. J Surg Res. 2008. PMID: 18155248
-
Postconditioning in focal cerebral ischemia: role of the mitochondrial ATP-dependent potassium channel.Brain Res. 2011 Feb 23;1375:137-46. doi: 10.1016/j.brainres.2010.12.054. Epub 2010 Dec 20. Brain Res. 2011. PMID: 21182830
-
Ischemic postconditioning as a novel avenue to protect against brain injury after stroke.J Cereb Blood Flow Metab. 2009 May;29(5):873-85. doi: 10.1038/jcbfm.2009.13. Epub 2009 Feb 25. J Cereb Blood Flow Metab. 2009. PMID: 19240739 Free PMC article. Review.
-
Effects of ischemic postconditioning and long non-coding RNAs in ischemic stroke.Bioengineered. 2022 Jun;13(6):14799-14814. doi: 10.1080/21655979.2022.2108266. Bioengineered. 2022. PMID: 36420646 Free PMC article. Review.
Cited by
-
Remote ischemic postconditioning promotes the survival of retinal ganglion cells after optic nerve injury.J Mol Neurosci. 2013 Nov;51(3):639-46. doi: 10.1007/s12031-013-0036-2. Epub 2013 Jun 5. J Mol Neurosci. 2013. PMID: 23733254
-
Bcl-2 phosphorylation triggers autophagy switch and reduces mitochondrial damage in limb remote ischemic conditioned rats after ischemic stroke.Transl Stroke Res. 2015 Jun;6(3):198-206. doi: 10.1007/s12975-015-0393-y. Epub 2015 Mar 7. Transl Stroke Res. 2015. PMID: 25744447
-
A critical review of mechanisms regulating remote preconditioning-induced brain protection.J Appl Physiol (1985). 2015 Nov 15;119(10):1135-42. doi: 10.1152/japplphysiol.00169.2015. Epub 2015 May 7. J Appl Physiol (1985). 2015. PMID: 25953834 Free PMC article. Review.
-
Ischemia-reperfusion injury: molecular mechanisms and therapeutic targets.Signal Transduct Target Ther. 2024 Jan 8;9(1):12. doi: 10.1038/s41392-023-01688-x. Signal Transduct Target Ther. 2024. PMID: 38185705 Free PMC article. Review.
-
Neuroprotective effects of bilobalide on cerebral ischemia and reperfusion injury are associated with inhibition of pro-inflammatory mediator production and down-regulation of JNK1/2 and p38 MAPK activation.J Neuroinflammation. 2014 Sep 26;11:167. doi: 10.1186/s12974-014-0167-6. J Neuroinflammation. 2014. PMID: 25256700 Free PMC article.
References
-
- Burda J, Danielisova V, Nemethova M, Gottlieb M, Matiasova M, Domorakova I, Mechirova E, Ferikova M, Salinas M, Burda R. Delayed postconditioning initiates additive mechanism necessary for survival of selectively vulnerable neurons after transient ischemia in rat brain. Cell Mol Neurobiol. 2006;26:1141–1151. - PMC - PubMed
-
- Dong HL, Zhang Y, Su BX, Zhu ZH, Gu QH, Sang HF, Xiong L. Limb remote ischemic preconditioning protects the spinal cord from ischemia-reperfusion injury: a newly identified nonneuronal but reactive oxygen species-dependent pathway. Anesthesiology. 2010;112:881–891. - PubMed
-
- Garcia JH, Liu KF, Ye ZR, Gutierrez JA.1997Incomplete infarct and delayed neuronal death after transient middle cerebral artery occlusion in rats Stroke 282303–2309.2310 - PubMed
-
- Gritsopoulos G, Iliodromitis EK, Zoga A, Farmakis D, Demerouti E, Papalois A, Paraskevaidis IA, Kremastinos DT. Remote postconditioning is more potent than classic postconditioning in reducing the infarct size in anesthetized rabbits. Cardiovasc Drugs Ther. 2009;23:193–198. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

