Vital-dye enhanced fluorescence imaging of GI mucosa: metaplasia, neoplasia, inflammation
- PMID: 22301343
- PMCID: PMC3336371
- DOI: 10.1016/j.gie.2011.10.004
Vital-dye enhanced fluorescence imaging of GI mucosa: metaplasia, neoplasia, inflammation
Abstract
Background: Confocal endomicroscopy has revolutionized endoscopy by offering subcellular images of the GI epithelium; however, the field of view is limited. Multiscale endoscopy platforms that use widefield imaging are needed to better direct the placement of high-resolution probes.
Design: Feasibility study.
Objective: This study evaluated the feasibility of a single agent, proflavine hemisulfate, as a contrast medium during both widefield and high-resolution imaging to characterize the morphologic changes associated with a variety of GI conditions.
Setting: The University of Texas MD Anderson Cancer Center, Houston, Texas, and Mount Sinai Medical Center, New York, New York. PATIENTS, INTERVENTIONS, AND MAIN OUTCOME MEASUREMENTS: Resected specimens were obtained from 15 patients undergoing EMR, esophagectomy, or colectomy. Proflavine hemisulfate, a vital fluorescent dye, was applied topically. The specimens were imaged with a widefield multispectral microscope and a high-resolution microendoscope. The images were compared with histopathologic examination.
Results: Widefield fluorescence imaging enhanced visualization of morphology, including the presence and spatial distribution of glands, glandular distortion, atrophy, and crowding. High-resolution imaging of widefield abnormal areas revealed that neoplastic progression corresponded to glandular heterogeneity and nuclear crowding in dysplasia, with glandular effacement in carcinoma. These widefield and high-resolution image features correlated well with the histopathologic features.
Limitations: This imaging approach must be validated in vivo with a larger sample size.
Conclusions: Multiscale proflavine-enhanced fluorescence imaging can delineate epithelial changes in a variety of GI conditions. Distorted glandular features seen with widefield imaging could serve as a critical bridge to high-resolution probe placement. An endoscopic platform combining the two modalities with a single vital dye may facilitate point-of-care decision making by providing real-time, in vivo diagnoses.
Copyright © 2012 American Society for Gastrointestinal Endoscopy. Published by Mosby, Inc. All rights reserved.
Figures


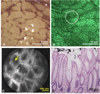



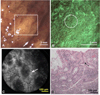

References
-
- Rubin DT, Rothe JA, Hetzel JT, Cohen RD, Hanauer SB. Are dysplasia and colorectal cancer endoscopically visible in patients with ulcerative colitis? Gastrointestinal Endoscopy. 2007;65:998–1004. - PubMed
-
- Vieth M, Ell C, Gossner L, May A, Stolte M. Histological analysis of endoscopic resection specimens from 326 patients with Barrett's esophagus and early neoplasia. Endoscopy. 2004;36:776–781. - PubMed
-
- Dekker E, van den Broek FJ, Reitsma JB, Hardwick JC, Offerhaus GJ, van Deventer SJ, Hommes DW, Fockens P. Narrow-band imaging compared with conventional colonoscopy for the detection of dysplasia in patients with longstanding ulcerative colitis. Endoscopy. 2007;39:216–221. - PubMed
-
- van den Broek FJ, Fockens P, van Eeden S, Reitsma JB, Hardwick JC, Stokkers PC, Dekker E. Endoscopic tri-modal imaging for surveillance in ulcerative colitis: randomised comparison of high-resolution endoscopy and autofluorescence imaging for neoplasia detection; and evaluation of narrow-band imaging for classification of lesions. Gut. 2008;57:1083–1089. - PMC - PubMed
-
- Kiesslich R, Burg J, Vieth M, Gnaendiger J, Enders M, Delaney P, Polglase A, McLaren W, Janell D, Thomas S, Nafe B, Galle PR, Neurath MF. Confocal laser endoscopy for diagnosing intraepithelial neoplasias and colorectal cancer in vivo. Gastroenterology. 2004;127:706–713. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

