Zinc and liver disease
- PMID: 22307488
- PMCID: PMC6027651
- DOI: 10.1177/0884533611433534
Zinc and liver disease
Erratum in
- Nutr Clin Pract. 2012 Apr;27(2):305. Mohommad, Mohammad K [corrected to Mohammad, Mohammad K]
Abstract
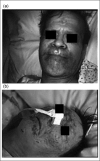
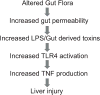
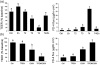
Zinc is an essential trace element required for normal cell growth, development, and differentiation. It is involved in DNA synthesis, RNA transcription, and cell division and activation. It is a critical component in many zinc protein/enzymes, including critical zinc transcription factors. Zinc deficiency/altered metabolism is observed in many types of liver disease, including alcoholic liver disease (ALD) and viral liver disease. Some of the mechanisms for zinc deficiency/altered metabolism include decreased dietary intake, increased urinary excretion, activation of certain zinc transporters, and induction of hepatic metallothionein. Zinc deficiency may manifest itself in many ways in liver disease, including skin lesions, poor wound healing/liver regeneration, altered mental status, or altered immune function. Zinc supplementation has been documented to block/attenuate experimental ALD through multiple processes, including stabilization of gut-barrier function, decreasing endotoxemia, decreasing proinflammatory cytokine production, decreasing oxidative stress, and attenuating apoptotic hepatocyte death. Clinical trials in human liver disease are limited in size and quality, but it is clear that zinc supplementation reverses clinical signs of zinc deficiency in patients with liver disease. Some studies suggest improvement in liver function in both ALD and hepatitis C following zinc supplementation, and 1 study suggested improved fibrosis markers in hepatitis C patients. The dose of zinc used for treatment of liver disease is usually 50 mg of elemental zinc taken with a meal to decrease the potential side effect of nausea.
Figures

References
-
- Vallee BL, Wacker WEC, Bartholomay AF, Robin ED. Zinc metabolism in hepatic dysfunction, I: serum zinc concentrations in Laennec’s cirrhosis and their validation by sequential analysis. N Engl J Med. 1956;255:403–408. - PubMed
-
- Vallee BL, Wacker WEC, Batholomay AF, Hoch FL. Zinc metabolism in hepatic dysfunction, II: correlation of metabolic patterns with biochemical findings. N Engl J Med. 1956;257:1056–1065. - PubMed
-
- Kahn AM, Helwig HL, Redeker AG, Reynolds TB. Urine and serum zinc abnormalities in disease of the liver. Am J Clin Pathol. 1965;44:426–435. - PubMed
-
- Sullivan JF, Heaney RP. Zinc metabolism in alcoholic liver disease. Am J Clin Nutr. 1970;23:170–177. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

