Effects of positive airway pressure therapy on neurobehavioral outcomes in children with obstructive sleep apnea
- PMID: 22323303
- PMCID: PMC3359938
- DOI: 10.1164/rccm.201112-2167OC
Effects of positive airway pressure therapy on neurobehavioral outcomes in children with obstructive sleep apnea
Abstract
Rationale: Positive airway pressure therapy is frequently used to treat obstructive sleep apnea in children. However, it is not known whether positive airway pressure therapy results in improvements in the neurobehavioral abnormalities associated with childhood sleep apnea.
Objectives: We hypothesized that positive airway pressure therapy would be associated with improvements in attention, sleepiness, behavior, and quality of life, and that changes would be associated with therapy adherence.
Methods: Neurobehavioral assessments were performed at baseline and after 3 months of positive airway pressure therapy in a heterogeneous group of 52 children and adolescents.
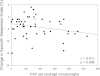
Measurements and main results: Adherence varied widely (mean use, 170 ± 145 [SD] minutes per night). Positive airway pressure therapy was associated with significant improvements in attention deficits (P < 0.001); sleepiness on the Epworth Sleepiness Scale (P < 0.001); behavior (P < 0.001); and caregiver- (P = 0.005) and child- (P < 0.001) reported quality of life. There was a significant correlation between the decrease in Epworth Sleepiness Scale at 3 months and adherence (r = 0.411; P = 0.006), but not between other behavioral outcomes and adherence. Behavioral factors also improved in the subset of children with developmental delays.
Conclusions: These results indicate that, despite suboptimal adherence use, there was significant improvement in neurobehavioral function in children after 3 months of positive airway pressure therapy, even in developmentally delayed children. The implications for improved family, social, and school function are substantial. Clinical trial registered with www.clinicaltrials.gov (NCT 00458406).
Trial registration: ClinicalTrials.gov NCT00458406.
Figures

Comment in
-
Investing in the future: the benefits of continuous positive airway pressure for childhood obstructive sleep apnea.Am J Respir Crit Care Med. 2012 May 1;185(9):908-10. doi: 10.1164/rccm.201202-0296ED. Am J Respir Crit Care Med. 2012. PMID: 22550207 No abstract available.
References
-
- American Academy of Pediatrics Clinical practice guideline: diagnosis and management of childhood obstructive sleep apnea syndrome. Pediatrics 2002;109:704–712 - PubMed
-
- Bhattacharjee R, Kheirandish-Gozal L, Spruyt K, Mitchell RB, Promchiarak J, Simakajornboon N, Kaditis AG, Splaingard D, Splaingard M, Brooks LJ, et al. Adenotonsillectomy outcomes in treatment of obstructive sleep apnea in children: a multicenter retrospective study. Am J Respir Crit Care Med 2010;182:676–683 - PubMed
-
- Beebe DW. Neurobehavioral morbidity associated with disordered breathing during sleep in children: a comprehensive review. Sleep 2006;29:1115–1134 - PubMed
-
- Difeo N, Meltzer LJ, Karamessinis L, Beck SE, Davis K, Schultz B, Samuel J, Traylor J, Marcus CL, et al. Effects of positive airway pressure (PAP) on neurobehavioral function in children. Sleep 2009;32:A87
Publication types
MeSH terms
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

