Increased gut microbial translocation in HIV-infected children persists in virologic responders and virologic failures after antiretroviral therapy
- PMID: 22333700
- PMCID: PMC3648848
- DOI: 10.1097/INF.0b013e31824da0f5
Increased gut microbial translocation in HIV-infected children persists in virologic responders and virologic failures after antiretroviral therapy
Abstract
Background: Gut microbial translocation (MT) is considered a major cause of immune activation (IA) and failure of immune reconstitution in HIV infection. This study investigated the relationship of virus replication, IA, CD4 counts and MT in HIV-infected children.
Methods: Lipopolysaccharide, bacterial 16S ribosomal DNA (16SrDNA) and soluble CD14 (sCD14) levels were determined in prospectively collected, stored plasma samples from the Pediatric AIDS Clinical Trials Group Protocol P338, a 48-week study initiated in 1997 to compare efficacy of dual nucleosides with a ritonavir-containing regimen. Results of MT were correlated with study data for T cell IA, plasma viral load and CD4 counts in 85 HIV-infected children (ages 2-17 years) designated as virologic responders or virologic failures (VF) at week 44 based on a cutoff of 400 HIV RNA copies/mL.
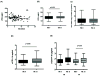
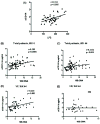
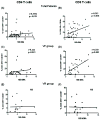
Results: Levels of plasma lipopolysaccharide, 16SrDNA and sCD14 were increased in comparison with HIV-uninfected controls and did not decrease at week 44 even in virologic responders. T cell IA was correlated with viral load and sCD14 at entry and with 16SrDNA and sCD14 at week 44 in total patients and in the VF group. Changes in 16SrDNA correlated with changes in IA and negatively with changes in CD4 counts. 16SrDNA was correlated with sCD14 but not with lipopolysaccharide.
Conclusions: MT persists after 44 weeks of antiretroviral therapy in VS and VF patients. In VF, 16SrDNA exhibited relationships to monocyte and T cell IA and CD4 counts but not with viral load, suggesting a dominant role for MT in disease pathogenesis in HIV-infected children.
Conflict of interest statement
Figures


References
-
- Liu Z, Cumberland WG, Hultin LE, Prince HE, Detels R, Giorgi JV. Elevated CD38 antigen expression on CD8+ T cells is a stronger marker for the risk of chronic HIV disease progression to AIDS and death in the Multicenter AIDS Cohort Study than CD4+ cell count, soluble immune activation markers, or combinations of HLA-DR and CD38 expression. J Acquir Immune Defic Syndr Hum Retrovirol. 1997;16:83–92. - PubMed
-
- Lederman MM, Kalish LA, Asmuth D, Fiebig E, Mileno M, Busch MP. ‘Modeling’ relationships among HIV-1 replication, immune activation and CD4+ T-cell losses using adjusted correlative analyses. AIDS. 2000;14:951–958. - PubMed
-
- Hazenberg MD, Otto SA, van Benthem BH, Roos MT, Coutinho RA, Lange JM, et al. Persistent immune activation in HIV-1 infection is associated with progression to AIDS. AIDS. 2003;17:1881–1888. - PubMed
-
- Deeks SG, Kitchen CM, Liu L, Guo H, Gascon R, Narvaez AB, et al. Immune activation set point during early HIV infection predicts subsequent CD4+ T-cell changes independent of viral load. Blood. 2004;104:942–947. - PubMed
-
- Brenchley JM, Price DA, Schacker TW, Asher TE, Silvestri G, Rao S, et al. Microbial translocation is a cause of systemic immune activation in chronic HIV infection. Nat Med. 2006;12:1365–1371. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

