Effect of T-cell-epitope matching at HLA-DPB1 in recipients of unrelated-donor haemopoietic-cell transplantation: a retrospective study
- PMID: 22340965
- PMCID: PMC3813000
- DOI: 10.1016/S1470-2045(12)70004-9
Effect of T-cell-epitope matching at HLA-DPB1 in recipients of unrelated-donor haemopoietic-cell transplantation: a retrospective study
Erratum in
- Lancet Oncol. 2012 Apr;13(4):e134-5
Abstract
Background: The risks after unrelated-donor haemopoietic-cell transplantation with matched HLA-A, HLA-B, HLA-C, HLA-DRB1, HLA-DQB1 alleles between donor and recipient (10/10 matched) can be decreased by selection of unrelated donors who also match for HLA-DPB1; however, such donors are difficult to find. Classification of HLA-DPB1 mismatches based on T-cell-epitope groups could identify mismatches that might be tolerated (permissive) and those that would increase risks (non-permissive) after transplantation. We did a retrospective study to compare outcomes between permissive and non-permissive HLA-DPB1 mismatches in unrelated-donor haemopoietic-cell transplantation.
Methods: HLA and clinical data for unrelated-donor [corrected] transplantations submitted to the International Histocompatibility Working Group in haemopoietic-cell transplantation were analysed retrospectively. HLA-DPB1 T-cell-epitope groups were assigned according to a functional algorithm based on alloreactive T-cell crossreactivity patterns. Recipients and unrelated donors matching status were classified as HLA-DPB1 match, non-permissive HLA-DPB1 mismatch (those with mismatched T-cell-epitope groups), or permissive HLA-DPB1 mismatch (those with matched T-cell-epitope groups). The clinical outcomes assessed were overall mortality, non-relapse mortality, relapse, and severe (grade 3-4) acute graft-versus-host disease (aGvHD).
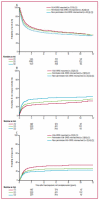
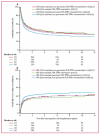
Findings: Of 8539 transplantations, 5428 (64%) were matched for ten of ten HLA alleles (HLA 10/10 matched) and 3111 (36%) for nine of ten alleles (HLA 9/10 matched). Of the group overall, 1719 (20%) were HLA-DPB1 matches, 2670 (31%) non-permissive HLA-DPB1 mismatches, and 4150 (49%) permissive HLA-DPB1 mismatches. In HLA 10/10-matched transplantations, non-permissive mismatches were associated with a significantly increased risk of overall mortality (hazard ratio [HR] 1·15, 95% CI 1·05-1·25; p=0·002), non-relapse mortality (1·28, 1·14-1·42; p<0·0001), and severe aGvHD (odds ratio [OR] 1·31, 95% CI 1·11-1·54; p=0·001), but not relapse (HR 0·89, 95% CI 0·77-1·02; p=0·10), compared with permissive mismatches. There were significant differences between permissive HLA-DPB1 mismatches and HLA-DPB1 matches in terms of non-relapse mortality (0·86, 0·75-0·98; p=0·03) and relapse (1·34, 1·17-1·54; p<0·0001), but not for overall mortality (0·96, 0·87-1·06; p=0·40) or aGvHD (OR 0·84, 95% CI 0·69-1·03; p=0·09). In the HLA 9/10 matched population, non-permissive HLA-DPB1 mismatches also increased the risk of overall mortality (HR 1·10, 95% CI 1·00-1·22; p=0·06), non-relapse mortality (1·19, 1·05-1·36; p=0·007), and severe aGvHD (OR 1·37, 95% CI 1·13-1·66; p=0·002) compared with permissive mismatches, but the risk of relapse was the same in both groups (HR 0·93, 95% CI 0·78-1·11; p=0·44). Outcomes for HLA 10/10-matched transplantations with non-permissive HLA-DPB1 mismatches did not differ substantially from those for HLA 9/10-matched transplantations with permissive HLA-DPB1 mismatches or HLA-DPB1 matches.
Interpretation: T-cell-epitope matching defines permissive and non-permissive HLA-DPB1 mismatches. Avoidance of an unrelated donor with a non-permissive T-cell-epitope mismatch at HLA-DPB1 might provide a practical clinical strategy for lowering the risks of mortality after unrelated-donor haemopoietic-cell transplantation.
Funding: National Institutes of Health; Associazione Italiana per la Ricerca sul Cancro; Telethon Foundation; Italian Ministry of Health; Cariplo Foundation; National Cancer Institute; National Heart, Lung and Blood Institute; National Institute of Allergy and Infectious Diseases; Office of Naval Research; IRGHET Paris; Swedish Cancer Society; Children's Cancer Foundation; Swedish Research Council; Cancer Society in Stockholm; Karolinska Institutet; and Leukemia and Lymphoma Society.
Copyright © 2012 Elsevier Ltd. All rights reserved.
Figures
Comment in
-
Permissive mismatches for blood and marrow transplantation.Lancet Oncol. 2012 Apr;13(4):323-4. doi: 10.1016/S1470-2045(12)70071-2. Epub 2012 Feb 15. Lancet Oncol. 2012. PMID: 22340963 No abstract available.
References
-
- Jeng RR, van den Brink MR. Allogeneic haematopoietic stem cell transplantation: individualized stem cell and immune therapy of cancer. Nat Rev Cancer. 2010;10:231–21. - PubMed
-
- Lee SJ, Klein J, Haagenson M, et al. High-resolution donor-recipient HLA matching contributes to the success of unrelated donor marrow transplantation. Blood. 2007;110:4576–83. - PubMed
-
- Morishima Y, Sasazuki T, Inoko H, et al. The clinical significance of human leukocyte antigen (HLA) allele compatibility in patients receiving a marrow transplant from serologically HLA-A, HLA-B, and HLA-DR matched unrelated donors. Blood. 2002;99:4200–06. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

