Differential effects of nebivolol and metoprolol on insulin sensitivity and plasminogen activator inhibitor in the metabolic syndrome
- PMID: 22353614
- PMCID: PMC3402551
- DOI: 10.1161/HYPERTENSIONAHA.111.189589
Differential effects of nebivolol and metoprolol on insulin sensitivity and plasminogen activator inhibitor in the metabolic syndrome
Abstract
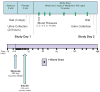
Early-generation β-blockers lower blood pressure and reduce cardiovascular morality in coronary artery disease and congestive heart failure but worsen glucose homeostasis and fibrinolytic balance. Nebivolol is a third-generation β-blocker that increases the bioavailability of nitric oxide. We compared the effect of nebivolol (5 mg/d) and the β(1)-selective antagonist metoprolol (100 mg/d) on glucose homeostasis and markers of fibrinolysis in 46 subjects with metabolic syndrome. Subjects underwent a frequently sampled IV glucose tolerance test after 3-week washout and placebo treatment and after randomized treatment with study drug. After 12-week treatment, nebivolol and metoprolol equivalently decreased systolic blood pressure, diastolic blood pressure, and heart rate. Neither drug affected β-cell function, disposition index, or acute insulin response to glucose. Metoprolol significantly decreased the insulin sensitivity index. In contrast, nebivolol did not affect insulin sensitivity, and the decrease in sensitivity was significantly greater after metoprolol than after nebivolol (-1.5±2.5×10(-4)×min(-1) per milliunit per liter versus 0.04±2.19×10(-4)×min(-1) per milliunit per liter after nebivolol; P=0.03). Circulating plasminogen activator inhibitor also increased after treatment with metoprolol (from 9.8±6.8 to 12.3±7.8 ng/mL) but not nebivolol (from 10.8±7.8 to 10.5±6.2 ng/mL; P=0.05 versus metoprolol). Metoprolol, but not nebivolol, increased F(2)-isoprostane concentrations. In summary, treatment with metoprolol decreased insulin sensitivity and increased oxidative stress and the antifibrinolytic plasminogen activator inhibitor 1 in patients with metabolic syndrome, whereas nebivolol lacked detrimental metabolic effects. Large clinical trials are needed to compare effects of nebivolol and the β(1) receptor antagonist metoprolol on clinical outcomes in patients with hypertension and the metabolic syndrome.
Trial registration: ClinicalTrials.gov NCT00775671.
Figures
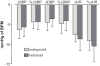
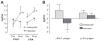
Similar articles
-
Cardiovascular protective effects of nebivolol in Zucker diabetic fatty rats.J Hypertens. 2010 May;28(5):1007-19. doi: 10.1097/hjh.0b013e328337598c. J Hypertens. 2010. PMID: 20411618
-
A comparison of the beta1-selectivity of three beta1-selective beta-blockers.J Clin Pharm Ther. 2003 Jun;28(3):179-86. doi: 10.1046/j.1365-2710.2003.00477.x. J Clin Pharm Ther. 2003. PMID: 12795776 Clinical Trial.
-
Comparative effects of nebivolol and metoprolol on oxidative stress, insulin resistance, plasma adiponectin and soluble P-selectin levels in hypertensive patients.J Hypertens. 2006 Mar;24(3):591-6. doi: 10.1097/01.hjh.0000209993.26057.de. J Hypertens. 2006. PMID: 16467663 Clinical Trial.
-
Metabolic profile of nebivolol, a beta-adrenoceptor antagonist with unique characteristics.Drugs. 2007;67(8):1097-107. doi: 10.2165/00003495-200767080-00001. Drugs. 2007. PMID: 17521213 Review.
-
Nebivolol: a novel beta-blocker with nitric oxide-induced vasodilatation.Vasc Health Risk Manag. 2006;2(3):303-8. doi: 10.2147/vhrm.2006.2.3.303. Vasc Health Risk Manag. 2006. PMID: 17326335 Free PMC article. Review.
Cited by
-
Effect of carvedilol versus nebivolol on insulin resistance among non-diabetic, non-ischemic cardiomyopathy with heart failure.Egypt Heart J. 2020 Sep 29;72(1):63. doi: 10.1186/s43044-020-00099-5. Egypt Heart J. 2020. PMID: 32990863 Free PMC article.
-
Fenofibrate lowers blood pressure in salt-sensitive but not salt-resistant hypertension.J Hypertens. 2013 Apr;31(4):820-9. doi: 10.1097/HJH.0b013e32835e8227. J Hypertens. 2013. PMID: 23385647 Free PMC article. Clinical Trial.
-
[Austrian Consensus on High Blood Pressure 2019].Wien Klin Wochenschr. 2019 Nov;131(Suppl 6):489-590. doi: 10.1007/s00508-019-01565-0. Wien Klin Wochenschr. 2019. PMID: 31792659 German.
-
The Pathophysiology and Treatment of Hypertension in Patients With Cushing's Syndrome.Front Endocrinol (Lausanne). 2019 May 21;10:321. doi: 10.3389/fendo.2019.00321. eCollection 2019. Front Endocrinol (Lausanne). 2019. PMID: 31164868 Free PMC article. Review.
-
Rationale for nebivolol/valsartan combination for hypertension: review of preclinical and clinical data.J Hypertens. 2017 Sep;35(9):1758-1767. doi: 10.1097/HJH.0000000000001412. J Hypertens. 2017. PMID: 28509722 Free PMC article. Review.
References
-
- Wang YC, McPherson K, Marsh T, Gortmaker SL, Brown M. Health and economic burden of the projected obesity trends in the USA and the UK. Lancet. 2011;378:815–825. - PubMed
-
- Lakka HM, Laaksonen DE, Lakka TA, Niskanen LK, Kumpusalo E, Tuomilehto J, Salonen JT. The metabolic syndrome and total and cardiovascular disease mortality in middle-aged men. JAMA. 2002;288:2709–2716. - PubMed
-
- Ingelsson E, Pencina MJ, Tofler GH, Benjamin EJ, Lanier KJ, Jacques PF, Fox CS, Meigs JB, Levy D, Larson MG, Selhub J, D’Agostino RB, Sr, Wang TJ, Vasan RS. Multimarker approach to evaluate the incidence of the metabolic syndrome and longitudinal changes in metabolic risk factors: the Framingham Offspring Study. Circulation. 2007;116:984–992. - PubMed
-
- Grant PJ. Diabetes mellitus as a prothrombotic condition. J Intern Med. 2007;262:157–172. - PubMed
-
- Scheen AJ. Prevention of type 2 diabetes mellitus through inhibition of the Renin-Angiotensin system. Drugs. 2004;64:2537–2565. - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

