Ultrasound-guided percutaneous endovascular aneurysm repair success is predicted by access vessel diameter
- PMID: 22360918
- PMCID: PMC3358509
- DOI: 10.1016/j.jvs.2011.12.042
Ultrasound-guided percutaneous endovascular aneurysm repair success is predicted by access vessel diameter
Abstract
Objective: Ultrasound scan-guided access allows for direct visualization of the access artery during percutaneous endovascular aortic aneurysm repair. We hypothesized that the use of ultrasound scan guidance allowed us to safely increase the utilization of percutaneous endovascular aortic aneurysm repair to almost all patients and decrease access complications.
Methods: A retrospective chart review of all elective endovascular aortic aneurysm repairs, both abdominal and descending thoracic, from 2005 to 2010 was performed. Patients were identified using International Classification of Disease, 9th Revision, Clinical Modification Codes and stratified based on access type: percutaneous vs cut-down. We examined the success rate of percutaneous access and the cause of failure. Sheath size was large (18-24 F) or small (12-16 F). Minimum access vessel diameter was also measured. Outcomes were wound complications (infections or clinically significant hematomas that delayed discharge or required transfusion), operative and incision time, length of stay, and discharge disposition. Predictors of percutaneous failure were identified.
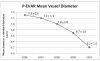
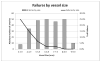
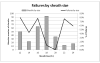
Results: One hundred sixty-eight patients (296 arteries) had percutaneous access endovascular aneurysm repair (P-EVAR) whereas 131 patients (226 arteries) had femoral cutdown access EVAR. Ultrasound scan-guided access was introduced in 2007. P-EVAR increased from zero cases in 2005 to 92.3% of all elective cases in 2010. The success rate with percutaneous access was 96%. Failures requiring open surgical repair of the artery included seven for hemorrhage and six for flow-limiting stenosis or occlusion of the femoral artery. P-EVAR had fewer wound complications (0.7% vs 7.4%; P = .001), shorter operative time (153.3 vs 201.5 minutes; P < .001), and larger minimal access vessel diameter (6.7 mm vs 6.1 mm; P < .01). Patients with failed percutaneous access had smaller minimal access vessel diameters when compared to successful P-EVAR (4.9 mm vs 6.8 mm; P < .001). More failures occurred in small sheaths than large ones (7.4% vs 1.9%; P = .02). Access vessel diameter <5 mm is predictive of percutaneous failure (16.7% of vessels <5 mm failed vs 2.4% of vessels ≥ 5 mm failed; P < .001; odds ratio, 7.3; 95% confidence interval, 1.58-33.8; P = .01).
Conclusions: Ultrasound scan-guided P-EVAR can be performed in the vast majority of patients with a high success rate, shorter operative times, and fewer wound complications. Access vessel diameters <5 mm are at greater risk for percutaneous failure and should be treated selectively.
Copyright © 2012 Society for Vascular Surgery. Published by Mosby, Inc. All rights reserved.
Figures




Similar articles
-
Preoperative risk score for access site failure in ultrasound-guided percutaneous aortic procedures.J Vasc Surg. 2019 Oct;70(4):1254-1262.e1. doi: 10.1016/j.jvs.2018.12.025. Epub 2019 Mar 7. J Vasc Surg. 2019. PMID: 30852039 Free PMC article.
-
The Kaiser Permanente experience with ultrasound-guided percutaneous endovascular abdominal aortic aneurysm repair.Ann Vasc Surg. 2012 Oct;26(7):906-12. doi: 10.1016/j.avsg.2011.09.013. Epub 2012 Apr 24. Ann Vasc Surg. 2012. PMID: 22534260
-
Impact of iliac artery anatomy on the outcome of fenestrated and branched endovascular aortic repair.J Vasc Surg. 2017 Dec;66(6):1659-1667. doi: 10.1016/j.jvs.2017.04.063. Epub 2017 Sep 6. J Vasc Surg. 2017. PMID: 28888759
-
Percutaneous versus femoral cutdown access for endovascular aneurysm repair.J Vasc Surg. 2015 Jul;62(1):16-21. doi: 10.1016/j.jvs.2015.01.058. Epub 2015 Mar 28. J Vasc Surg. 2015. PMID: 25827969 Free PMC article.
-
Surgical outcomes and indications for saccular abdominal aortic aneurysm repair: a systematic review.J Vasc Bras. 2025 May 30;24:e20240164. doi: 10.1590/1677-5449.202401642. eCollection 2025. J Vasc Bras. 2025. PMID: 40487735 Free PMC article. Review.
Cited by
-
Initial experience with polymer endovascular aneurysm repair using the Alto stent graft.J Vasc Surg Cases Innov Tech. 2020 Feb 1;6(1):6-11. doi: 10.1016/j.jvscit.2019.04.007. eCollection 2020 Mar. J Vasc Surg Cases Innov Tech. 2020. PMID: 32025596 Free PMC article.
-
Percutaneous thoracic endovascular aortic repair is not contraindicated in obese patients.J Vasc Surg. 2014 Oct;60(4):921-8. doi: 10.1016/j.jvs.2014.04.051. Epub 2014 May 17. J Vasc Surg. 2014. PMID: 24845111 Free PMC article.
-
Preoperative risk score for access site failure in ultrasound-guided percutaneous aortic procedures.J Vasc Surg. 2019 Oct;70(4):1254-1262.e1. doi: 10.1016/j.jvs.2018.12.025. Epub 2019 Mar 7. J Vasc Surg. 2019. PMID: 30852039 Free PMC article.
-
A comparison of Percutaneous femoral access in Endovascular Repair versus Open femoral access (PiERO): study protocol for a randomized controlled trial.Trials. 2015 Sep 14;16:408. doi: 10.1186/s13063-015-0911-y. Trials. 2015. PMID: 26370286 Free PMC article. Clinical Trial.
-
Total percutaneous femoral vessels cannulation for minimally invasive mitral valve surgery.Ann Cardiothorac Surg. 2013 Nov;2(6):739-43. doi: 10.3978/j.issn.2225-319X.2013.08.02. Ann Cardiothorac Surg. 2013. PMID: 24349975 Free PMC article.
References
-
- Haas PC, Krajcer Z, Diethrich EB. Closure of large percutaneous access sites using the Prostar XL Percutaneous Vascular Surgery device. J Endovasc Surg. 1999;6(2):168–170. - PubMed
-
- Howell M, Villareal R, Krajcer Z. Percutaneous access and closure of femoral artery access sites associated with endoluminal repair of abdominal aortic aneurysms. J Endovasc Ther. 2001;8(1):68–74. - PubMed
-
- Lee WA, Brown MP, Nelson PR, Huber TS. Total percutaneous access for endovascular aortic aneurysm repair (“Preclose” technique) J Vasc Surg. 2007;45(6):1095–1101. - PubMed
-
- Quinn SF, Kim J. Percutaneous femoral closure following stent-graft placement: use of the Perclose device. Cardiovasc Intervent Radiol. 2004;27(3):231–236. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

