Toxicities of immunosuppressive treatment of autoimmune neurologic diseases
- PMID: 22379461
- PMCID: PMC3151601
- DOI: 10.2174/157015911796557939
Toxicities of immunosuppressive treatment of autoimmune neurologic diseases
Abstract
In parallel to our better understanding of the role of the immune system in neurologic diseases, there has been an increased availability in therapeutic options for autoimmune neurologic diseases such as multiple sclerosis, myasthenia gravis, polyneuropathies, central nervous system vasculitides and neurosarcoidosis. In many cases, the purported benefits of this class of therapy are anecdotal and not the result of good controlled clinical trials. Nonetheless, their potential efficacy is better known than their adverse event profile. A rationale therapeutic decision by the clinician will depend on a comprehensive understanding of the ratio between efficacy and toxicity. In this review, we outline the most commonly used immune suppressive medications in neurologic disease: cytotoxic chemotherapy, nucleoside analogues, calcineurin inhibitors, monoclonal antibodies and miscellaneous immune suppressants. A discussion of their mechanisms of action and related toxicity is highlighted, with the goal that the reader will be able to recognize the most commonly associated toxicities and identify strategies to prevent and manage problems that are expected to arise with their use.
Keywords: Immunosuppressive therapy; auto-immune neurologic disease.; toxicity.
Figures
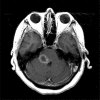
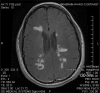
References
-
- Guyton AC, Hall JE. Textbook of Medical Physiology. 11th. Philadelphia, PA: Saunders; 2005.
-
- Weiner HL, Cohen JA. Treatment of multiple sclerosis with cyclophosphamide: critical review of clinical and immunologic effects. Mult. Scler. 2002;8(2):142–54. - PubMed
-
- Korkmaz A, Topal T, Oter S. Pathophysiological aspects of cyclophosphamide and ifosfamide induced hemorrhagic cystitis; implication of reactive oxygen and nitrogen species as well as PARP activation. Cell Biol.Toxicol. 2007;23(5):303–12. - PubMed
-
- Virag L, Szabo E, Gergely P, Szabo C. Peroxynitrite-induced cytotoxicity: mechanism and opportunities for intervention. Toxicol. Lett. 2003;140-141:113–24. - PubMed
LinkOut - more resources
Full Text Sources
