Low-frequency electrotherapy for female patients with detrusor underactivity due to neuromuscular deficiency
- PMID: 22441580
- PMCID: PMC3396337
- DOI: 10.1007/s00192-012-1714-2
Low-frequency electrotherapy for female patients with detrusor underactivity due to neuromuscular deficiency
Abstract
Introduction and hypothesis: The aim of the study was to assess the efficacy of low-frequency electrotherapy (LFE) for female patients with early-stage detrusor underactivity (DUA) due to neuromuscular deficiency.
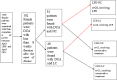
Methods: A total of 102 female patients were divided randomly into four groups: LFE-NC (normal compliance), LFE-LC (low compliance), CON (control)-NC and CON-LC. Patients in the LFE-NC and LFE-LC groups received LFE, and those in the CON-NC and CON-LC groups received conservative treatment. Urodynamic evaluation was performed before and after treatment.
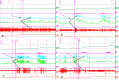
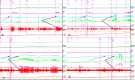
Results: After treatment, 82 % of the LFE-NC regained detrusor contractility, whereas only 2 (8 %) of the CON-NC had normal detrusor contraction. None of LFE-LC or CON-LC regained detrusor contractility (p < 0.01). The per cent of LFE-NC who relied on catheterization for bladder emptying decreased by 43 % (p < 0.01). Those in the LFE-LC, CON-NC and CON-LC groups decreased by only 4, 12 or 0 % (p > 0.05).
Conclusions: LFE was more effective for DUA patients with normal compliance; these patients benefited from LFE, but DUA patients with low compliance did not.
Figures
Similar articles
-
Contemporary concepts in the aetiopathogenesis of detrusor underactivity.Nat Rev Urol. 2014 Nov;11(11):639-48. doi: 10.1038/nrurol.2014.286. Epub 2014 Oct 21. Nat Rev Urol. 2014. PMID: 25330789 Review.
-
Proposal for a urodynamic redefinition of detrusor underactivity.J Urol. 2009 Jan;181(1):225-9. doi: 10.1016/j.juro.2008.09.018. Epub 2008 Nov 14. J Urol. 2009. PMID: 19013594
-
Detrusor underactivity and the underactive bladder: a new clinical entity? A review of current terminology, definitions, epidemiology, aetiology, and diagnosis.Eur Urol. 2014 Feb;65(2):389-98. doi: 10.1016/j.eururo.2013.10.015. Epub 2013 Oct 26. Eur Urol. 2014. PMID: 24184024 Review.
-
Investigation of urodynamic characteristics and bladder sensory function in the early stages of diabetic bladder dysfunction in women with type 2 diabetes.J Urol. 2009 Jan;181(1):198-203. doi: 10.1016/j.juro.2008.09.021. Epub 2008 Nov 14. J Urol. 2009. PMID: 19013605
-
The natural history of lower urinary tract dysfunction in men: minimum 10-year urodynamic follow-up of untreated detrusor underactivity.BJU Int. 2005 Dec;96(9):1295-300. doi: 10.1111/j.1464-410X.2005.05891.x. BJU Int. 2005. PMID: 16287448
Cited by
-
Relationship between urodynamic patterns and lower urinary tract symptoms in Chinese women with a non-neurogenic bladder.Asian J Urol. 2016 Jan;3(1):10-19. doi: 10.1016/j.ajur.2015.11.004. Epub 2015 Dec 2. Asian J Urol. 2016. PMID: 29264157 Free PMC article.
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

