Splint: the efficacy of orthotic management in rest to prevent equinus in children with cerebral palsy, a randomised controlled trial
- PMID: 22448907
- PMCID: PMC3328267
- DOI: 10.1186/1471-2431-12-38
Splint: the efficacy of orthotic management in rest to prevent equinus in children with cerebral palsy, a randomised controlled trial
Abstract
Background: Range of motion deficits of the lower extremity occur in about the half of the children with spastic cerebral palsy (CP). Over time, these impairments can cause joint deformities and deviations in the children's gait pattern, leading to limitations in moblity. Preventing a loss of range of motion is important in order to reduce secondary activity limitations and joint deformities. Sustained muscle stretch, imposed by orthotic management in rest, might be an effective method of preventing a decrease in range of motion. However, no controlled study has been performed.
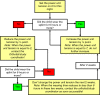
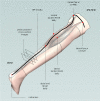
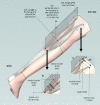
Methods: A single blind randomised controlled trial will be performed in 66 children with spastic CP, divided over three groups with each 22 participants. Two groups will be treated for 1 year with orthoses to prevent a decrease in range of motion in the ankle (either with static or dynamic knee-ankle-foot-orthoses) and a third group will be included as a control group and will receive usual care (physical therapy, manual stretching). Measurements will be performed at baseline and at 3, 6, 9 and 12 months after treatment allocation. The primary outcome measure will be ankle dorsiflexion at full knee extension, measured with a custom designed hand held dynamometer. Secondary outcome measures will be i) ankle and knee flexion during gait and ii) gross motor function. Furthermore, to gain more insight in the working mechanism of the orthotic management in rest, morphological parameters like achilles tendon length, muscle belly length, muscle fascicle length, muscle physiological cross sectional area length and fascicle pennation angle will be measured in a subgroup of 18 participants using a 3D imaging technique.
Discussion: This randomised controlled trial will provide more insight into the efficacy of orthotic management in rest and the working mechanisms behind this treatment. The results of this study could lead to improved treatments.
Trial registration number: Nederlands Trial Register NTR2091.
Figures





References
-
- Rosenbaum P, Paneth N, Leviton A, Goldstein M, Bax M, Damiano D, Dan B, Jacobsson B. A report: the definition and classification of cerebral palsy April 2006. Dev Med Child Neurol Suppl. 2007;109:8–14. - PubMed
-
- McManus V, Guillem P, Surman G, Cans C. SCPE work, standardization and definition-an overview of the activities of SCPE: a collaboration of European CP registers. Zhongguo Dang Dai Er Ke Za Zhi. 2006;8:261–265. - PubMed
-
- Lance JW. In: Spasticity: disordered motor control. Feldman RG, Young RR, KW, editor. Miami: Year Book Medical Publishers; 1980. Symposium synopsis; pp. 485–500.
-
- Himmelmann K, Hagberg G, Beckung E, Hagberg B, Uvebrant P. The changing panorama of cerebral palsy in Sweden. IX. Prevalence and origin in the birth-year period 1995-1998. Acta Paediatr. 2005;94:287–294. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

