Distinct roles of trauma and transfusion in induction of immune modulation after injury
- PMID: 22452342
- PMCID: PMC3392528
- DOI: 10.1111/j.1537-2995.2012.03618.x
Distinct roles of trauma and transfusion in induction of immune modulation after injury
Abstract
Background: Trauma and transfusion can both alter immunity, and while transfusions are common among traumatically injured patients, few studies have examined their combined effects on immunity.
Study design and methods: We tracked the plasma levels of 41 immunomodulatory proteins in 56 trauma patients from time of injury up to 1 year later. In addition, a murine model was developed to distinguish between the effects of transfusion and underlying injury and blood loss.
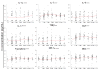
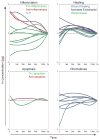
Results: Thirty-one of the proteins had a significant change over time after traumatic injury, with a mixed early response that was predominantly anti-inflammatory followed by a later increase in proteins involved in wound healing and homeostasis. Results from the murine model revealed similar cytokine responses to humans. In mice, trauma and hemorrhage caused early perturbations in a number of the pro- and anti-inflammatory mediators measured, and transfusion blunted early elevations in interleukin (IL)-6, IL-10, matrix metalloproteinase-9, and interferon-γ. Transfusion caused or exacerbated changes in monocyte chemotactic protein-1, IL-1α, IL-5, IL-15, and soluble E-selectin. Finally, trauma and hemorrhage alone increased CXCL1 and IL-13.
Conclusions: This work provides a detailed characterization of the major shift in the immunologic environment in response to trauma and transfusion and clarifies which immune mediators are affected by trauma and hemorrhage and which by transfusion.
© 2012 American Association of Blood Banks.
Conflict of interest statement
Competing interests: the authors have no competing interests.
Figures





References
-
- Trunkey DD. History and development of trauma care in the United States. Clin Orthop Relat Res. 2000:36–46. - PubMed
-
- Como JJ, Dutton RP, Scalea TM, Edelman BB, Hess JR. Blood transfusion rates in the care of acute trauma. Transfusion. 2004;44:809–13. - PubMed
-
- Department of Health and Human Services U. The 2009 National Blood Collection and Utilization Survey Report. 2009.
-
- Giannoudis PV. Current concepts of the inflammatory response after major trauma: an update. Injury. 2003;34:397–404. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases
Research Materials

