Groove pancreatitis: A Case Report and Review of the Literature
- PMID: 22470697
- PMCID: PMC3303357
- DOI: 10.3941/jrcr.v4i11.588
Groove pancreatitis: A Case Report and Review of the Literature
Abstract
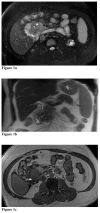
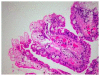
Groove pancreatitis is a rare form of segmental chronic pancreatitis. It involves the anatomic space between the head of the pancreas, the duodenum and the common bile duct. It was first described in the early 1970s, but it remains largely unfamiliar to most physicians. Radiological diagnosis can be challenging, as it is often difficult to differentiate it from other entities. The differential diagnosis from pancreatic head carcinoma may be difficult and recognition of subtle differences between these two entities is extremely important as the management differs significantly. Groove pancreatitis can be managed by conservative medical treatment, and surgery is reserved only for patients with persistent and severe clinical symptoms. We present a case of a 27 year-old male with groove pancreatitis and discuss the Magnetic Resonance Imaging (MRI) appearance of this entity as well as the differential diagnosis.
Keywords: Chronic pancreatitis; Groove pancreatitis; MRI; Magnetic Resonance Imaging.
Figures


References
-
- Ishigami K, Tajima T, Nishie A, et al. Differential diagnosis of groove pancreatic carcinomas vs. groove pancreatitis: Usefulness of the portal venous phase. Eur J Radiol. 2010;74:e95–e100. - PubMed
-
- Graziani R, Tapparelli M, Malago R, et al. The various imaging aspects of chronic pancreatitis. JOP. 2005;6:73–88. - PubMed
-
- Levenick JM, Gordon SR, Sutton JE, Suriawinata A, Gardner TB. A comprehensive, case-based review of groove pancreatitis. Pancreas. 2009;38:e169–175. - PubMed
-
- Shanbhogue AK, Fasih N, Surabhi VR, Doherty GP, Shanbhogue DK, Sethi SK. A clinical and radiologic review of uncommon types and causes of pancreatitis. RadioGraphics. 2009;29:1003–1026. - PubMed
-
- Stolte M, Weiss W, Volkholz H, Rosch W. A special form of segmental pancreatitis: “groove pancreatitis”. Hepatogastroenterology. 1982;29:198–208. - PubMed
LinkOut - more resources
Full Text Sources