Clinical use of multifocal visual-evoked potentials in a glaucoma practice: a prospective study
- PMID: 22476612
- PMCID: PMC3498911
- DOI: 10.1007/s10633-012-9324-3
Clinical use of multifocal visual-evoked potentials in a glaucoma practice: a prospective study
Abstract
Purpose: To test a framework that describes how the multifocal visual-evoked potential (mfVEP) technique is used in a particular glaucoma practice.
Methods: In this prospective, descriptive study, glaucoma suspects, ocular hypertensives and glaucoma patients were referred for mfVEP testing by a single glaucoma specialist over a 2-year period. All patients underwent standard automated perimetry (SAP) and mfVEP testing within 3 months. Two hundred and ten patients (420 eyes) were referred for mfVEP testing for the following reasons: (1) normal SAP tests suspected of early functional loss (ocular hypertensives, n = 43; and glaucoma suspects on the basis of suspicious optic disks, n = 52); (2) normal-tension glaucoma patients with suspected central SAP defects (n = 33); and (3) SAP abnormalities needing confirmation (n = 82).
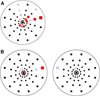
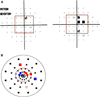
Results: All the glaucoma suspects with normal SAP and mfVEP results remained untreated. Of those with abnormal mfVEP results, 68 % (15/22) were treated because the abnormal regions on the mfVEP were consistent with the abnormal regions seen during clinical examination of the optic disk. The mfVEP was abnormal in 86 % (69/80) of eyes with glaucomatous optic neuropathy and SAP damage, even though it did not result in an altered treatment regimen. In NTG patients, the mfVEP showed central defects in 44 % (12 of 27) of the eyes with apparently normal central fields and confirmed central scotomata in 92 % (36 of 39), leading to more rigorous surveillance of these patients.
Conclusions: In a clinical practice, the mfVEP was used when clinical examination and subjective visual fields provided insufficient or conflicting information. This information influenced clinical management.
Conflict of interest statement
Figures



Similar articles
-
Comparing multifocal VEP and standard automated perimetry in high-risk ocular hypertension and early glaucoma.Invest Ophthalmol Vis Sci. 2007 Mar;48(3):1173-80. doi: 10.1167/iovs.06-0561. Invest Ophthalmol Vis Sci. 2007. PMID: 17325161
-
Evaluation of the visual function in obstructive sleep apnea syndrome patients and normal-tension glaucoma by means of the multifocal visual evoked potentials.Graefes Arch Clin Exp Ophthalmol. 2012 Nov;250(11):1681-8. doi: 10.1007/s00417-012-1982-z. Epub 2012 Mar 14. Graefes Arch Clin Exp Ophthalmol. 2012. PMID: 22411129
-
Effect of recording duration on the diagnostic performance of multifocal visual-evoked potentials in high-risk ocular hypertension and early glaucoma.J Glaucoma. 2008 Apr-May;17(3):175-82. doi: 10.1097/IJG.0b013e31815678ac. J Glaucoma. 2008. PMID: 18414101 Free PMC article.
-
[New insights into the pathogenesis of glaucomatous optic neuropathy and refinement of the objective assessment of its functional damage].Nippon Ganka Gakkai Zasshi. 2012 Mar;116(3):298-344; discussion 345-6. Nippon Ganka Gakkai Zasshi. 2012. PMID: 22568105 Review. Japanese.
-
Multifocal VEP and ganglion cell damage: applications and limitations for the study of glaucoma.Prog Retin Eye Res. 2003 Mar;22(2):201-51. doi: 10.1016/s1350-9462(02)00061-7. Prog Retin Eye Res. 2003. PMID: 12604058 Review.
Cited by
-
Multifocal visual evoked potential for evaluation of open-angle glaucoma.Med Hypothesis Discov Innov Ophthalmol. 2021 Nov 17;10(3):114-120. doi: 10.51329/mehdiophthal1429. eCollection 2021 Fall. Med Hypothesis Discov Innov Ophthalmol. 2021. PMID: 37641709 Free PMC article.
-
Structural and Functional Evaluations for the Early Detection of Glaucoma.Expert Rev Ophthalmol. 2016;11(5):367-376. doi: 10.1080/17469899.2016.1229599. Epub 2016 Sep 14. Expert Rev Ophthalmol. 2016. PMID: 28603546 Free PMC article.
-
Comparing three different modes of electroretinography in experimental glaucoma: diagnostic performance and correlation to structure.Doc Ophthalmol. 2017 Apr;134(2):111-128. doi: 10.1007/s10633-017-9578-x. Epub 2017 Feb 27. Doc Ophthalmol. 2017. PMID: 28243926 Free PMC article.
-
Structural and functional changes in glaucoma: comparing the two-flash multifocal electroretinogram to optical coherence tomography and visual fields.Doc Ophthalmol. 2015 Jun;130(3):197-209. doi: 10.1007/s10633-015-9482-1. Epub 2015 Jan 24. Doc Ophthalmol. 2015. PMID: 25616700
References
-
- Shah NN, Bowd C, Medeiros FA, Weinreb RN, Sample PA, Hoffmann EM, Zangwill LM. Combining structural and functional testing for detection of glaucoma. Ophthalmology. 2006;113:1593–1602. - PubMed
-
- Nouri-Mahdavi K, Hoffman D, Tannenbaum DP, Law SK, Caprioli J. Identifying early glaucoma with optical coherence tomography. Am J Ophthalmol. 2004;137:228–235. - PubMed
-
- Reus NJ, Lemij HJ. The relationship between standard automated perimetry and GDx VCC measurements. Invest Ophthalmol Vis Sci. 2004;45:840–845. - PubMed
-
- Reus NJ, Lemij HJ. Relationships between standard automated perimetry, HRT confocal scanning laser ophthalmoscopy, and GDx VCC scanning laser polarimetry. Invest Ophthalmol Vis Sci. 2005;46:4182–4188. - PubMed
-
- Bowd C, Zangwill LM, Medeiros FA, Tavares IM, Hoffmann EM, Bourne RR, Sample PA, Weinreb RN. Structure-function relationships using confocal scanning laser ophthalmoscopy, optical coherence tomography, and scanning laser polarimetry. Invest Ophthalmol Vis Sci. 2006;47:2889–2895. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

