Achalasia--a disease of unknown cause that is often diagnosed too late
- PMID: 22532812
- PMCID: PMC3329145
- DOI: 10.3238/arztebl.2012.0209
Achalasia--a disease of unknown cause that is often diagnosed too late
Abstract
Introduction: Many physicians are inadequately familiar with the clinical features of achalasia. Often, it is not diagnosed until years after the symptoms arise. This is unfortunate, because a delay in diagnosis worsens the prognosis.
Methods: Selective review of the literature.
Results: Achalasia has a lifetime prevalence of 1:10 000. It is a neurodegenerative disorder in which the neurons of the myenteric plexus are lost, leading to dysfunction of the lower esophageal sphincter and to a derangement of esophageal peristalsis. In the final stage of achalasia, esophageal motility is irreversibly impaired, and complications ensue because of the retention of food that is no longer transported into the stomach. Aspiration causes pulmonary disturbances in up to half of all patients with achalasia. There may also be inflammation of the esophageal mucosa (retention esophagitis); this, in turn, is a risk factor for esophageal cancer, which arises in 4% to 6% of patients. The cause of achalasia is not fully known, but autoimmune processes appear to be involved in patients with a genetic susceptibility to the disease.
Conclusion: Achalasia should be diagnosed as early as possible, so that complications can be prevented. In addition, guidelines should be established for cancer prevention in achalasia patients. Currently ongoing studies of the molecular causes of achalasia will probably help us understand its pathophysiology.
Figures

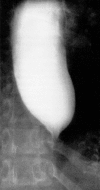

Comment in
-
Two arguments in favor of surgery.Dtsch Arztebl Int. 2012 Aug;109(31-32):534. doi: 10.3238/arztebl.2012.0534a. Epub 2012 Aug 6. Dtsch Arztebl Int. 2012. PMID: 23049649 Free PMC article. No abstract available.
-
No new therapeutic approach.Dtsch Arztebl Int. 2012 Aug;109(31-32):534. doi: 10.3238/arztebl.2012.0534b. Epub 2012 Aug 6. Dtsch Arztebl Int. 2012. PMID: 23049650 Free PMC article. No abstract available.
References
-
- Park W, Vaezi MF. Etiology and pathogenesis of achalasia: the current understanding. Am J Gastroenterol. 2005;100:1404–1414. - PubMed
-
- Gockel HR, Schumacher J, Gockel I, Lang H, Haaf T, Nothen MM. Achalasia: will genetic studies provide insights? Hum Genet. 2010;128:353–364. - PubMed
-
- Vela MF, Vaezi MF. Cost-assessment of alternative management strategies for achalasia. Expert Opin Pharmacother. 2003;4:2019–2025. - PubMed
-
- Eckardt VF. Clinical presentations and complications of achalasia. Gastrointest Endosc Clin N Am. 2001;11:281–292. - PubMed
-
- Eckardt VF, Kohne U, Junginger T, Westermeier T. Risk factors for diagnostic delay in achalasia. Dig Dis Sci. 1997;42:580–585. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

