Positron emission tomography for assessing local failure after stereotactic body radiotherapy for non-small-cell lung cancer
- PMID: 22572078
- PMCID: PMC3474601
- DOI: 10.1016/j.ijrobp.2011.10.035
Positron emission tomography for assessing local failure after stereotactic body radiotherapy for non-small-cell lung cancer
Abstract
Purpose: We analyzed whether positron emission tomography (PET)/computed tomography standardized uptake values (SUVs) after stereotactic body radiotherapy (SBRT) could predict local recurrence (LR) in non-small-cell lung cancer (NSCLC).
Methods and materials: This study comprised 128 patients with Stage I (n = 68) or isolated recurrent/secondary parenchymal (n = 60) NSCLC treated with image-guided SBRT to 50 Gy over 4 consecutive days; prior radiotherapy was allowed. PET/computed tomography scans were obtained before therapy and at 1 to 6 months after therapy, as well as subsequently as clinically indicated. Continuous variables were analyzed with Kruskal-Wallis tests and categorical variables with Pearson chi-square or Fisher exact tests. Actuarial local failure rates were calculated with the Kaplan-Meier method.
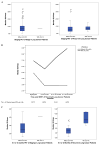
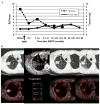
Results: At a median follow-up of 31 months (range, 6-71 months), the actuarial 1-, 2-, and 3-year local control rates were 100%, 98.5%, and 98.5%, respectively, in the Stage I group and 95.8%, 87.6%, and 85.8%, respectively, in the recurrent group. The cumulative rates of regional nodal recurrence and distant metastasis were 8.8% (6 of 68) and 14.7% (10 of 68), respectively, for the Stage I group and 11.7% (7 of 60) and 16.7% (10 of 60), respectively, for the recurrent group. Univariate analysis showed that SUVs obtained 12.1 to 24 months after treatment for the Stage I group (p = 0.007) and 6.1 to 12 months and 12.1 to 24 months after treatment for the recurrent group were associated with LR (p < 0.001 for both). Of the 128 patients, 17 (13.3%) had ipsilateral consolidation after SBRT but no elevated metabolic activity on PET; none had LR. The cutoff maximum SUV of 5 was found to have 100% sensitivity, 91% specificity, a 50% positive predictive value, and a 100% negative predictive value for predicting LR.
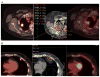
Conclusions: PET was helpful for distinguishing SBRT-induced consolidation from LR. SUVs obtained more than 6 months after SBRT for NSCLC were associated with local failure. A maximum SUV greater than 5, especially at more than 6 months after SBRT, should prompt biopsy to rule out LR.
Copyright © 2012 Elsevier Inc. All rights reserved.
Conflict of interest statement
Conflict of interest: none.
Figures
References
-
- Jemal A, Siegel R, Ward E, et al. Cancer statistics, 2009. CA Cancer J Clin. 2009;59:225–249. - PubMed
-
- Rami-Porta R, Ball D, Crowley J, et al. The IASLC lung cancer staging project: Proposals for the revision of the T descriptors in the forthcoming (seventh) edition of the TNM classification for lung cancer. J Thorac Oncol. 2007;2:593–602. - PubMed
-
- Bach PB, Cramer LD, Warren JL, et al. Racial differences in the treatment of early-stage lung cancer. N Engl J Med. 1999;341:1198–1205. - PubMed
-
- Onishi H, Araki T, Shirato H, et al. Stereotactic hypofractionated high-dose irradiation for stage I non-small cell lung carcinoma clinical outcome in 245 subjects in a Japanese multiinstitutional study. Cancer. 2004;101:1623–1631. - PubMed
-
- Timmerman R, McGarry R, Yiannoutsos C, et al. Excessive toxicity when treating central tumors in a phase II study of stereotactic body radiation therapy for medically inoperable early-stage lung cancer. J Clin Oncol. 2006;24:4833–4839. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

