3.0 T MRI of 2000 consecutive patients with localisation-related epilepsy
- PMID: 22573303
- PMCID: PMC3487054
- DOI: 10.1259/bjr/30177037
3.0 T MRI of 2000 consecutive patients with localisation-related epilepsy
Abstract
Objectives: Clinical guidelines suggest that all patients diagnosed with localised seizures should be investigated with MRI to identify any epileptogenic structural lesions, as these patients may benefit from surgical resection. There is growing impetus to use higher field strength scanners to image such patients, as some evidence suggests that they improve detection rates. We set out to review the detection rate of radiological abnormalities found by imaging patients with localised seizures using a high-resolution 3.0 T epilepsy protocol.
Methods: Data were reviewed from 2000 consecutive adult patients with localisation-related epilepsy referred between January 2005 and February 2011, and imaged at 3.0 T using a standard epilepsy protocol.
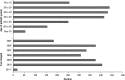
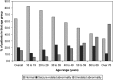
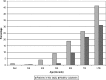
Results: An abnormality likely to be related to seizure activity was identified in 403/2000 (20.2%) patients, with mesial temporal sclerosis diagnosed in 211 patients. 313/2000 (15.6%) had lesions potentially amenable to surgery. Abnormalities thought unrelated to seizure activity were found in 324/2000 (16.1%), with 8.9% having evidence of ischaemic disease.
Conclusions: Since the introduction of the then National Institute for Clinical Excellence guidelines in 2004, the detection rate of significant pathology using a dedicated 3.0 T epilepsy protocol has not fallen, despite the increased numbers of patients being imaged. This is the largest study of epilepsy imaging at 3.0 T to date and highlights the detection rates of significant pathology in a clinical setting using a high-strength magnet. The prevalence of ischaemic disease in this population is significantly higher than first thought, and may not be incidental, as is often reported.
Figures

References
-
- Duncan JS. Imaging and epilepsy. Brain 1997;120:339–77 - PubMed
-
- Stokes T, Shaw E, Juarez-Garcia A, Camosso-Stefinovic J, Baker R. Clinical guidelines and evidence review for the epilepsies: diagnosis and management in adults and children in primary and secondary care. London, UK: Royal College of General Practitioners; 2004
-
- Commission on Neuroimaging of the International League Against Epilepsy Recommendations for neuroimaging of patients with epilepsy. Epilepsia 1997;38:1255–6 - PubMed
-
- Gaillard WD, Chiron C, Cross JH, Harvey AS, Kuzniecky R, Hertz-Pannier L, et al. Guidelines for imaging infants and children with recent-onset epilepsy. Epilepsia 2009;50:2147–53 - PubMed
-
- Sztriha L, Gururaj AK, Bener A, Nork M. Temporal lobe epilepsy in children: etiology in a cohort with new-onset seizures. Epilepsia 2002;43:75–80 - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

