Salvage liver transplantation is a reasonable option for selected patients who have recurrent hepatocellular carcinoma after liver resection
- PMID: 22574187
- PMCID: PMC3344909
- DOI: 10.1371/journal.pone.0036587
Salvage liver transplantation is a reasonable option for selected patients who have recurrent hepatocellular carcinoma after liver resection
Abstract
Background: Salvage liver transplantation (SLT) has been reported as being feasible for patients who develop recurrent hepatocellular carcinoma (HCC) after primary liver resection, but this finding remains controversial. We retrospectively studied the clinical characteristics of SLT recipients and conducted a comparison between SLT recipients and primary liver transplantation (PLT) recipients.
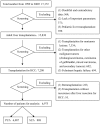
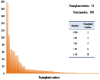
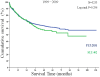
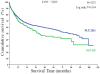
Methodology and principal findings: A retrospective study examined data from the China Liver Transplant Registry (CLTR) for 6,975 transplants performed from January 1999 to December 2009. A total of 6,087 patients underwent PLT and 888 patients underwent SLT for recurrence. Living donor liver transplantation (LDLT) was performed in 389 patients, while 6,586 patients underwent deceased donor liver transplantation (DDLT). Kaplan-Meier curves were used to compare survival rates. The 1-year, 3-year, and 5-year overall survival of SLT recipients was similar to that of PLT recipients: 73.00%, 51.77%, and 45.84% vs. 74.49%, 55.10%, and 48.81%, respectively (P = 0.260). The 1-year, 3-year and 5-year disease-free survival of SLT recipients was inferior to that of PLT recipients: 64.79%, 45.57%, and 37.78% vs. 66.39%, 50.39%, and 43.50%, respectively (P = 0.048). Similar survival results were observed for SLT and PLT within both the LDLT and DDLT recipients. Within the SLT group, the 1-year, 3-year, and 5-year overall survival for LDLT and DDLT recipients was similar: 93.33%, 74.67%, and 74.67% vs. 80.13%, 62.10%, and 54.18% (P = 0.281), as was the disease-free survival: 84.85%, 62.85%, and 62.85% vs. 70.54%, 53.94%, and 43.57% (P = 0.462).
Conclusions: Our study demonstrates that for selected patients, SLT has similar survival to that of PLT, indicating that SLT is acceptable for patients with recurrent HCC after liver resection. Given the limited organ donor pool, salvage LDLT might be considered as a possible treatment.
Conflict of interest statement
Figures
References
-
- Fan ST, Cheung ST, Lo CM. Indications for liver transplantation in patients with chronic hepatitis B and C virus infection and hepatocellular carcinoma. J Gastroenterol Hepatol. 2000;15(Suppl):E181–186. - PubMed
-
- Mor E, Kaspa RT, Sheiner P, Schwartz M. Treatment of hepatocellular carcinoma associated with cirrhosis in the era of liver transplantation. Ann Intern Med. 1998;129:643–653. - PubMed
-
- Mazzaferro V, Regalia E, Doci R, Andreola S, Pulvirenti A, et al. Liver transplantation for the treatment of small hepatocellular carcinomas in patients with cirrhosis. N Engl J Med. 1996;334:693–699. - PubMed
-
- Dmitrewski J, El-Gazzaz G, McMaster P. Hepatocellular cancer: resection or transplantation. J Hepatobiliary Pancreat Surg. 1998;5:18–23. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

