Reconstruction of scalp defects with the radial forearm free flap
- PMID: 22583845
- PMCID: PMC3414765
- DOI: 10.1186/1758-3284-4-21
Reconstruction of scalp defects with the radial forearm free flap
Expression of concern in
-
Comment: Head and Neck Oncology.BMC Med. 2014 Feb 5;12:24. doi: 10.1186/1741-7015-12-24. BMC Med. 2014. PMID: 24499430 Free PMC article. Review.
Abstract
Background: Advanced and recurrent cutaneous squamous cell carcinoma of the scalp and forehead require aggressive surgical excision often resulting in complex defects requiring reconstruction. This study evaluates various microvascular free flap reconstructions in this patient population, including the rarely utilized radial forearm free flap.
Patients and methods: A retrospective review of patients undergoing free flap surgeries (n = 47) of the scalp between 1997 and 2011 were included. Patients were divided primarily into two cohorts: a new primary lesion (n = 21) or recurrence (n = 26). Factors examined include patient demographics, indication for surgery, defect, type of flap used, complications (major and minor), and outcomes.
Results: The patients were primarily male (n = 34), with a mean age of 67 years (25-91). A total of 58 microvascular free flap reconstructions were performed (radial forearm free flap: n = 28, latissimus dorsi: n = 20, rectus abdominis: n = 9, scapula: n = 1). Following reconstruction with a radial forearm free flap, duration of hospitalization was shorter (P = 0.04) and complications rates were similar (P = 0.46). Donor site selection correlated with defect area (P < 0.001), but not with the extent of skull defect (P = 0.70). Larger defect areas correlated with higher complications rates (P = 0.03) and longer hospitalization (P = 0.003). Patients were more likely to require multiple reconstructions if referred for a recurrent lesions (P = 0.01) or received prior radiation therapy (P = 0.02).
Conclusion: Advanced and recurrent malignancies of the scalp are aggressive and challenging to treat. The radial forearm free flap is an underutilized free flap in the reconstruction of complex scalp defects.
Figures
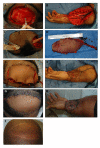
References
-
- Chang KP, Lai CH, Chang CH, Lin CL, Lai CS, Lin SD. Free flap options for reconstruction of complicated scalp and calvarial defects: report of a series of cases and literature review. Microsurgery. 2010;30:13–18. - PubMed
-
- Wang HT, Erdmann D, Olbrich KC, Friedman AH, Levin LS, Zenn MR. Free flap reconstruction of the scalp and calvaria of major neurosurgical resections in cancer patients: lessons learned closing large, difficult wounds of the dura and skull. Plast Reconstr Surg. 2007;119:865–872. doi: 10.1097/01.prs.0000240830.19716.c2. - DOI - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

