Doxycycline improves filarial lymphedema independent of active filarial infection: a randomized controlled trial
- PMID: 22610930
- PMCID: PMC3412691
- DOI: 10.1093/cid/cis486
Doxycycline improves filarial lymphedema independent of active filarial infection: a randomized controlled trial
Abstract
Background: The aim of this study was to determine whether improvement of filarial lymphedema (LE) by doxycycline is restricted to patients with ongoing infection (positive for circulating filarial antigen [CFA]), or whether the majority of CFA-negative patients with LE would also show a reduction in LE severity.
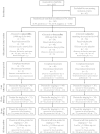
Methods: One hundred sixty-two Ghanaian participants with LE stage 1-5 (Dreyer) were randomized blockwise into 2 groups (CFA positive or negative) and allocated to 3 treatment arms of 6 weeks: (1) amoxicillin (1000 mg/d), (2) doxycycline (200 mg/d), or (3) placebo matching doxycycline. All groups received standard hygiene morbidity management. The primary outcome was reduction of LE stages. Secondary outcomes included frequency of acute attacks and ultrasonographic assessment of skin thickness at the ankles. Parameters were assessed before treatment and after 3, 12, and 24 months.
Results: Doxycycline-treated patients with LE stage 2-3 showed significant reductions in LE severity after 12 and 24 months, regardless of CFA status. Improvement was observed in 43.9% of doxycycline-treated patients, compared with only 3.2% and 5.6% in the amoxicillin and placebo arms, respectively. Skin thickness was correlated with LE stage improvement. Both doxycycline and amoxicillin were able to reduce acute dermatolymphangioadenitis attacks.
Conclusions: Doxycycline treatment improves mild to moderate LE independent of ongoing infection. This finding expands the benefits of doxycycline to the entire population of patients suffering from LE. Patients with LE stage 1-3 should benefit from a 6-week course of doxycycline every other year or yearly, which should be considered as an improved tool to manage morbidity in filarial LE. Clinical Trials Registration. ISRCTN 90861344.
Figures



References
-
- WHO. GPELF progress report 2000-2009 and strategic plan 2010–2020. Available at: http://www.who.int/neglected_diseases/integrated_media/integrated_media_.... Accessed 23 May 2012.
-
- Dreyer G, Medeiros Z, Netto MJ, Leal NC, de Castro LG, Piessens WF. Acute attacks in the extremities of persons living in an area endemic for bancroftian filariasis: differentiation of two syndromes. Trans R Soc Trop Med Hyg. 1999;93:413–7. - PubMed
-
- Dreyer G, Addiss D, Dreyer P, Noroes J. Basic lymphoedema management: treatment and prevention of problems associated with lymphatic filariasis. Hollis, NH: Hollis Publishing; 2002.
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

