Hemangiomas and vascular malformations: current theory and management
- PMID: 22611412
- PMCID: PMC3352592
- DOI: 10.1155/2012/645678
Hemangiomas and vascular malformations: current theory and management
Abstract
Vascular anomalies are a heterogeneous group of congenital blood vessel disorders more typically referred to as birthmarks. Subcategorized into vascular tumors and malformations, each anomaly is characterized by specific morphology, pathophysiology, clinical behavior, and management approach. Hemangiomas are the most common vascular tumor. Lymphatic, capillary, venous, and arteriovenous malformations make up the majority of vascular malformations. This paper reviews current theory and practice in the etiology, diagnosis, and treatment of these more common vascular anomalies.
Figures
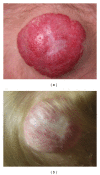
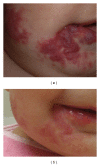
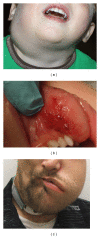
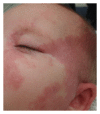

References
-
- Mulliken JB, Glowacki J. Hemangiomas and vascular malformations in infants and children: a classification based on endothelial characteristics. Plastic and Reconstructive Surgery. 1982;69(3):412–422. - PubMed
-
- Haggstrom AN, Drolet BA, Baselga E, et al. Prospective study of infantile hemangiomas: demographic, prenatal, and perinatal characteristics. Journal of Pediatrics. 2007;150(3):291–294. - PubMed
-
- North PE, Waner M, Brodsky MC. Are infantile hemangiomas of placental origin? Ophthalmology. 2002;109(4):633–634. - PubMed
-
- Yu Y, Flint AF, Mulliken JB, Wu JK, Bischoff J. Endothelial progenitor cells in infantile hemangioma. Blood. 2004;103(4):1373–1375. - PubMed
LinkOut - more resources
Full Text Sources

