Impact of hypertension on ventricular-arterial coupling and regional myocardial work at rest and during isometric exercise
- PMID: 22622108
- PMCID: PMC3607228
- DOI: 10.1016/j.echo.2012.04.018
Impact of hypertension on ventricular-arterial coupling and regional myocardial work at rest and during isometric exercise
Abstract
Background: To understand better the mechanism of left ventricular (LV) remodeling related to hypertension, it is important to evaluate LV function in relation to the changes in loading conditions. The aim of this study was to investigate changes in conventional ventricular-arterial coupling indexes, LV strain, and a new index reflecting regional myocardial work assessed noninvasively at rest and during isometric exercise in a random sample including participants with normal blood pressure and those with hypertension.
Methods: A total of 148 participants (53.4% women; mean age, 52.0 years; 39.2% with hypertension) underwent simultaneous echocardiographic and arterial data acquisition at rest and during increased afterload (handgrip exercise). End-systolic pressure was determined from the carotid pulse wave. Arterial elastance (Ea) and LV elastance (Ees) were calculated as end-systolic pressure/stroke volume and end-systolic pressure/end-systolic volume. Doppler tissue imaging and two-dimensional speckle tracking were used to derive LV longitudinal strain. Regional myocardial work (ejection work density [EWD]) was the area of the pressure-strain loop during ejection.
Results: At rest, with adjustments applied, Ees (3.06 vs 3.71 mm Hg/mL, P = .0003), Ea/Ees (0.54 vs 0.47, P = .002) and EWD (670 vs 802 Pa/m(2), P = .0001) differed significantly between participants with normal blood pressure and those with hypertension. During handgrip exercise, Ea and Ea/Ees significantly increased (P < .0001) in both groups. Doppler tissue imaging and two-dimensional LV strain decreased in participants with hypertension (P ≤ .008). Only in subjects with normal blood pressure EWD significantly increased (+14.7%, P = .0009).
Conclusions: Although patients with hypertension compared with those with normal blood pressure have increased LV systolic stiffness and regional myocardial work to match arterial load at rest, they might have diminished cardiac reserve to increase myocardial performance, as estimated by EWD during isometric exercise.
Copyright © 2012 American Society of Echocardiography. Published by Mosby, Inc. All rights reserved.
Figures


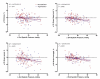
Comment in
-
Left ventricular function and the systemic arterial vasculature: remembering what we have learned.J Am Soc Echocardiogr. 2012 Aug;25(8):891-4. doi: 10.1016/j.echo.2012.06.020. J Am Soc Echocardiogr. 2012. PMID: 22824174 Free PMC article. No abstract available.
References
-
- Kass DA. Ventricular arterial stiffening: integrating the pathophysiology. Hypertension. 2005;46:185–93. - PubMed
-
- de Tombe PP, Jones S, Burkhoff D, Hunter WC, Kass DA. Ventricular stroke and efficiency both remain nearly optimal despite altered vascular loading. Am J Physiol. 1993;264:H1817–24. - PubMed
-
- Kawaguchi M, Hay I, Fetics BJ, Kass DA. Combined ventricular systolic and arterial stiffening in patients with heart failure and preserved ejection fraction: implications for systolic and diastolic reserve limitations. Circulation. 2003;107:714–20. - PubMed
-
- Sunagawa K, Sagawa K, Maughan WL. Ventriculo-vascular coupling: clinical, physiologic, and engineering aspects. Springer Verlag; New York: 1987. Ventricular interaction with the vascular system in terms of pressure-volumes relationships; pp. 210–39.
-
- Saba PS, Ganau A, Devereux RB, Pini R, Pickering TG, Roman MJ. Impact of arterial elastance as a measure of vascular load on left ventricular geometry in hypertension. J Hypertens. 1999;17:1007–15. - PubMed

