Molecular and cellular mechanisms of skeletal muscle atrophy: an update
- PMID: 22673968
- PMCID: PMC3424188
- DOI: 10.1007/s13539-012-0074-6
Molecular and cellular mechanisms of skeletal muscle atrophy: an update
Abstract
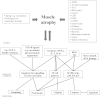
Skeletal muscle atrophy is defined as a decrease in muscle mass and it occurs when protein degradation exceeds protein synthesis. Potential triggers of muscle wasting are long-term immobilization, malnutrition, severe burns, aging as well as various serious and often chronic diseases, such as chronic heart failure, obstructive lung disease, renal failure, AIDS, sepsis, immune disorders, cancer, and dystrophies. Interestingly, a cooperation between several pathophysiological factors, including inappropriately adapted anabolic (e.g., growth hormone, insulin-like growth factor 1) and catabolic proteins (e.g., tumor necrosis factor alpha, myostatin), may tip the balance towards muscle-specific protein degradation through activation of the proteasomal and autophagic systems or the apoptotic pathway. Based on the current literature, we present an overview of the molecular and cellular mechanisms that contribute to muscle wasting. We also focus on the multifacetted therapeutic approach that is currently employed to prevent the development of muscle wasting and to counteract its progression. This approach includes adequate nutritional support, implementation of exercise training, and possible pharmacological compounds.
Figures
References
-
- Thomas DR. Loss of skeletal muscle mass in aging: examining the relationship of starvation, sarcopenia and cachexia. Clin Nutr. 2007;26:389–99. - PubMed
-
- Vandervoort AA. Aging of the human neuromuscular system. Muscle Nerve. 2002;25:17–25. - PubMed
-
- Dedkov EI, Borisov AB, Carlson BM. Dynamics of postdenervation atrophy of young and old skeletal muscles: differential responses of fiber types and muscle types. J Gerontol A Biol Sci Med Sci. 2003;58:984–91. - PubMed
-
- Williams AD, Selig S, Hare DL, Hayes A, Krum H, Patterson J, et al. Reduced exercise tolerance in CHF may be related to factors other than impaired skeletal muscle oxidative capacity. J Card Fail. 2004;10:141–8. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources