Effect of regression from prediabetes to normal glucose regulation on long-term reduction in diabetes risk: results from the Diabetes Prevention Program Outcomes Study
- PMID: 22683134
- PMCID: PMC3555407
- DOI: 10.1016/S0140-6736(12)60525-X
Effect of regression from prediabetes to normal glucose regulation on long-term reduction in diabetes risk: results from the Diabetes Prevention Program Outcomes Study
Abstract
Background: Our objective was to quantify and predict diabetes risk reduction during the Diabetes Prevention Program Outcomes Study (DPPOS) in participants who returned to normal glucose regulation at least once during the Diabetes Prevention Program (DPP) compared with those who consistently met criteria for prediabetes.
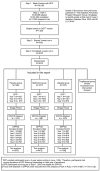
Methods: DPPOS is an ongoing observational study of participants from the DPP randomised trial. For this analysis, diabetes cumulative incidence in DPPOS was calculated for participants with normal glucose regulation or prediabetes status during DPP with and without stratification by previous randomised treatment group. Cox proportional hazards modelling and generalised linear mixed models were used to quantify the effect of previous (DPP) glycaemic status on risk of later (DPPOS) diabetes and normal glucose regulation status, respectively, per SD in change. Included in this analysis were 1990 participants of DPPOS who had been randomly assigned to treatment groups during DPP (736 intensive lifestyle intervention, 647 metformin, 607 placebo). These studies are registered at ClinicalTrials.gov, NCT00004992 (DPP) and NCT00038727 (DPPOS).
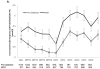
Findings: Diabetes risk during DPPOS was 56% lower for participants who had returned to normal glucose regulation versus those who consistently had prediabetes (hazard ratio [HR] 0·44, 95% CI 0·37-0·55, p<0·0001) and was unaffected by previous group assignment (interaction test for normal glucose regulation and lifestyle intervention, p=0·1722; normal glucose regulation and metformin, p=0·3304). Many, but not all, of the variables that increased diabetes risk were inversely associated with the chance of a participant reaching normal glucose regulation status in DPPOS. Specifically, previous achievement of normal glucose regulation (odds ratio [OR] 3·18, 95% CI 2·71-3·72, p<0·0001), increased β-cell function (OR 1·28; 95% CI 1·18-1·39, p<0·0001), and insulin sensitivity (OR 1·16, 95% CI 1·08-1·25, p<0·0001) were associated with normal glucose regulation in DPPOS, whereas the opposite was true for prediction of diabetes, with increased β-cell function (HR 0·80, 95% CI 0·71-0·89, p<0·0001) and insulin sensitivity (HR 0·83, 95% CI 0·74-0·94, p=0·0001) having a protective effect. Among participants who did not return to normal glucose regulation in DPP, those assigned to the intensive lifestyle intervention had a higher diabetes risk (HR 1·31, 95% CI 1·03-1·68, p=0·0304) and lower chance of normal glucose regulation (OR 0·59, 95% CI 0·42-0·82, p=0·0014) than did the placebo group in DPPOS.
Interpretation: We conclude that prediabetes is a high-risk state for diabetes, especially in patients who remain with prediabetes despite intensive lifestyle intervention. Reversion to normal glucose regulation, even if transient, is associated with a significantly reduced risk of future diabetes independent of previous treatment group.
Funding: US National Institutes of Health.
Copyright © 2012 Elsevier Ltd. All rights reserved.
Conflict of interest statement
The authors have no relevant conflicts of interest to disclose.
Figures



Comment in
-
Is regression to normoglycaemia clinically important?Lancet. 2012 Jun 16;379(9833):2216-8. doi: 10.1016/S0140-6736(12)60828-9. Epub 2012 Jun 9. Lancet. 2012. PMID: 22683127 No abstract available.
-
Diabetes: normal glucose levels should be the goal.Nat Rev Endocrinol. 2012 Sep;8(9):510-2. doi: 10.1038/nrendo.2012.139. Epub 2012 Jul 31. Nat Rev Endocrinol. 2012. PMID: 22847240 No abstract available.
-
[Prediabetes: high risk factor for diabetes mellitus type 2? - Successful prevention with early interventions for lifestyle modification].Dtsch Med Wochenschr. 2012 Sep;137(37):1788. doi: 10.1055/s-0032-1327078. Epub 2012 Sep 6. Dtsch Med Wochenschr. 2012. PMID: 22956217 German. No abstract available.
-
Reducing the risk of development of diabetes: do we have an answer?Natl Med J India. 2012 Jul-Aug;25(4):221-2. Natl Med J India. 2012. PMID: 23278780 No abstract available.
References
-
- CDC. Diabetes Fact Sheet online 2011. Jan 26, 2011.
-
- Ford ES, Zhao G, Li C. Pre-diabetes and the risk for cardiovascular disease: a systematic review of the evidence. J Am Coll Cardiol. 2010 Mar 30;55(13):1310–7. - PubMed
-
- Ziegler D, Rathmann W, Dickhaus T, Meisinger C, Mielck A. Prevalence of polyneuropathy in pre-diabetes and diabetes is associated with abdominal obesity and macroangiopathy: the MONICA/KORA Augsburg Surveys S2 and S3. Diabetes Care. 2008 Mar;31(3):464–9. - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

