A discrete population of squamocolumnar junction cells implicated in the pathogenesis of cervical cancer
- PMID: 22689991
- PMCID: PMC3387104
- DOI: 10.1073/pnas.1202684109
A discrete population of squamocolumnar junction cells implicated in the pathogenesis of cervical cancer
Abstract
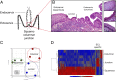
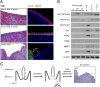
Infection by carcinogenic human papillomaviruses (HPV) results in precancers [cervical intraepithelial neoplasia (CIN)] and cancers near the ectoendocervical squamocolumnar (SC) junction of the cervix. However, the specific cells targeted by HPV have not been identified and the cellular origin of cervical cancer remains elusive. In this study, we uncovered a discrete population of SC junctional cells with unique morphology and gene-expression profile. We also demonstrated that the selected junctional biomarkers were expressed by a high percentage of high-grade CIN and cervical cancers associated with carcinogenic HPVs but rarely in ectocervical/transformation zone CINs or those associated with noncarcinogenic HPVs. That the original SC junction immunophenotype was not regenerated at new SC junctions following excision, not induced by expression of viral oncoproteins in foreskin keratinocytes, and not seen in HPV-related precursors of the vagina, vulva, and penis further support the notion that junctional cells are the source of cervical cancer. Taken together, our findings suggest that carcinogenic HPV-related CINs and cervical cancers are linked to a small, discrete cell population that localizes to the SC junction of the cervix, expresses a unique gene expression signature, and is not regenerated after excision. The findings in this study uncover a potential target for cervical cancer prevention, provide insight into the risk assessment of cervical lesions, and establish a model for elucidating the pathway to cervical cancer following carcinogenic HPV infection.
Conflict of interest statement
The authors declare no conflict of interest.
Figures


References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

