Nuclear nano-morphology markers of histologically normal cells detect the "field effect" of breast cancer
- PMID: 22706633
- PMCID: PMC3566261
- DOI: 10.1007/s10549-012-2125-2
Nuclear nano-morphology markers of histologically normal cells detect the "field effect" of breast cancer
Abstract
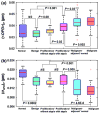
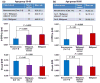
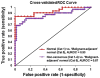
Accurate detection of breast malignancy from histologically normal cells ("field effect") has significant clinical implications in a broad base of breast cancer management, such as high-risk lesion management, personalized risk assessment, breast tumor recurrence, and tumor margin management. More accurate and clinically applicable tools to detect markers characteristic of breast cancer "field effect" that are able to guide the clinical management are urgently needed. We have recently developed a novel optical microscope, spatial-domain low-coherence quantitative phase microscopy, which extracts the nanoscale structural characteristics of cell nuclei (i.e., nuclear nano-morphology markers), using standard histology slides. In this proof-of-concept study, we present the use of these highly sensitive nuclear nano-morphology markers to identify breast malignancy from histologically normal cells. We investigated the nano-morphology markers from 154 patients with a broad spectrum of breast pathology entities, including normal breast tissue, non-proliferative benign lesions, proliferative lesions (without and with atypia), "malignant-adjacent" normal tissue, and invasive carcinoma. Our results show that the nuclear nano-morphology markers of "malignant-adjacent" normal tissue can detect the presence of invasive breast carcinoma with high accuracy and do not reflect normal aging. Further, we found that a progressive change in nuclear nano-morphology markers that parallel breast cancer risk, suggesting its potential use for risk stratification. These novel nano-morphology markers that detect breast cancerous changes from nanoscale structural characteristics of histologically normal cells could potentially benefit the diagnosis, risk assessment, prognosis, prevention, and treatment of breast cancer.
Conflict of interest statement
Figures



References
-
- Kopelovich L, Henson DE, Gazdar AF, Dunn B, Srivastava S, Kelloff GJ, Greenwald P. Surrogate anatomic/functional sites for evaluating cancer risk: an extension of the field effect. Clin Cancer Res. 1999;5(12):3899–3905. - PubMed
-
- Slaughter DP, Southwick HW, Smejkal W. Field cancerization in oral stratified squamous epithelium; clinical implications of multicentric origin. Cancer. 1953;6(5):963–968. - PubMed
-
- Chai H, Brown RE. Field effect in cancer-an update. Ann Clin Lab Sci. 2009;39(4):331–337. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

