Effects of anesthetic regimes on inflammatory responses in a rat model of acute lung injury
- PMID: 22711173
- PMCID: PMC4896809
- DOI: 10.1007/s00134-012-2610-4
Effects of anesthetic regimes on inflammatory responses in a rat model of acute lung injury
Abstract
Purpose: Gamma-aminobutyric acid (GABA) is the major inhibitory neurotransmitter through activation of GABA receptors. Volatile anesthetics activate type-A (GABA(A)) receptors resulting in inhibition of synaptic transmission. Lung epithelial cells have been recently found to express GABA(A) receptors that exert anti-inflammatory properties. We hypothesized that the volatile anesthetic sevoflurane (SEVO) attenuates lung inflammation through activation of lung epithelial GABA(A) receptors.
Methods: Sprague-Dawley rats were anesthetized with SEVO or ketamine/xylazine (KX). Acute lung inflammation was induced by intratracheal instillation of endotoxin, followed by mechanical ventilation for 4 h at a tidal volume of 15 mL/kg without positive end-expiratory pressure (two-hit lung injury model). To examine the specific effects of GABA, healthy human lung epithelial cells (BEAS-2B) were challenged with endotoxin in the presence and absence of GABA with and without addition of the GABA(A) receptor antagonist picrotoxin.
Results: Anesthesia with SEVO improved oxygenation and reduced pulmonary cytokine responses compared to KX. This phenomenon was associated with increased expression of the π subunit of GABA(A) receptors and glutamic acid decarboxylase (GAD). The endotoxin-induced cytokine release from BEAS-2B cells was attenuated by the treatment with GABA, which was reversed by the administration of picrotoxin.
Conclusion: Anesthesia with SEVO suppresses pulmonary inflammation and thus protects the lung from the two-hit injury. The anti-inflammatory effect of SEVO is likely due to activation of pulmonary GABA(A) signaling pathways.
Figures
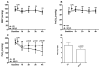



References
-
- Phua J, Badia JR, Adhikari NK, Friedrich JO, Fowler RA, Singh JM, Scales DC, Stather DR, Li A, Jones A, Gattas DJ, Hallett D, Tomlinson G, Stewart TE, Ferguson ND. Has mortality from acute respiratory distress syndrome decreased over time?: A systematic review. Am J Respir Crit Care Med. 2009;179:220–227. - PubMed
-
- The Acute Respiratory Distress Syndrome N. Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. N Engl J Med. 2000;342:1301–1308. - PubMed
-
- Brun-Buisson C, Minelli C, Bertolini G, Brazzi L, Pimentel J, Lewandowski K, Bion J, Romand J, Villar J, Thorsteinsson A, Damas P, Armaganidis A, Lemaire F for the ASG. Epidemiology and outcome of acute lung injury in European intensive care units. Results from the ALIVE study. Intensive Care Med. 2004;30:51–61. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

