Adaptive servoventilation for treatment of sleep-disordered breathing in heart failure: a systematic review and meta-analysis
- PMID: 22722232
- PMCID: PMC3494473
- DOI: 10.1378/chest.12-0815
Adaptive servoventilation for treatment of sleep-disordered breathing in heart failure: a systematic review and meta-analysis
Abstract
Background: Adaptive servoventilation (ASV) has demonstrated efficacy in treating sleep-disordered breathing (SDB) in patients with heart failure (HF), but large randomized trials are lacking. We, therefore, sought to perform a systematic review and meta-analysis of existing data.
Methods: A systematic search of the PubMed database was undertaken in March 2012. Publications were independently assessed by two investigators to identify studies of ≥ 1-week duration that compared ASV to a control condition (ie, subtherapeutic ASV, continuous or bilevel pressure ventilation, oxygen therapy, or no treatment) in adult patients with SDB and HF. Mean, variability,and sample size data were extracted independently for the following outcomes: apneahypopnea index (AHI), left ventricular ejection fraction (LVEF), quality of life (SF-36 Health Survey; Medical Outcomes Trust), 6-min walk distance, peak oxygen consumption ( VO 2 ) % predicted, and ventilatory equivalent ratio for CO 2 ( VE / Vco 2 ) slope measured during exercise. Random effects meta-analysis models were applied.
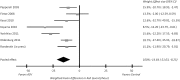
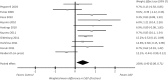
Results: Fourteen studies were identified (N = 538). Comparing ASV to control conditions, the weighted mean difference in AHI ( -14.64 events/h; 95% CI, -21.03 to - 8.25) and LVEF (0.40;95% CI, 0.08-0.71) both significantly favored ASV. ASV also improved the 6-min walk distance,but not peak O 2 % predicted, VE / VCO 2 slope, or quality of life, compared with control conditions.
Conclusions: In patients with HF and SDB, ASV was more effective than control conditions in reducing the AHI and improving cardiac function and exercise capacity. These data provide a compelling rationale for large-scale randomized controlled trials to assess the clinical impact of ASV on hard outcomes in these patients.
Figures
References
-
- Chan J, Sanderson J, Chan W, et al. Prevalence of sleep-disordered breathing in diastolic heart failure. Chest. 1997; 111(6):1488-1493 - PubMed
-
- Naughton MT, Benard DC, Liu PP, Rutherford R, Rankin F, Bradley TD. Effects of nasal CPAP on sympathetic activity in patients with heart failure and central sleep apnea. Am J Respir Crit Care Med. 1995; 152(2):473-479 - PubMed
-
- Granton JT, Naughton MT, Benard DC, Liu PP, Goldstein RS, Bradley TD. CPAP improves inspiratory muscle strength in patients with heart failure and central sleep apnea. Am J Respir Crit Care Med. 1996; 153(1):277-282 - PubMed
-
- Sin DD, Logan AG, Fitzgerald FS, Liu PP, Bradley TD. Effects of continuous positive airway pressure on cardiovascular outcomes in heart failure patients with and without Cheyne-Stokes respiration. Circulation. 2000; 102(1):61-66 - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases
Research Materials
Miscellaneous

