Inflammatory cytokines in experimental and human stroke
- PMID: 22739623
- PMCID: PMC3434626
- DOI: 10.1038/jcbfm.2012.88
Inflammatory cytokines in experimental and human stroke
Abstract
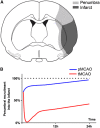
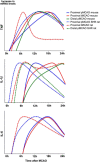
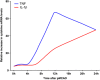
Inflammation is a hallmark of stroke pathology. The cytokines, tumor necrosis factor (TNF), interleukin (IL)-1, and IL-6, modulate tissue injury in experimental stroke and are therefore potential targets in future stroke therapy. The effect of these cytokines on infarct evolution depends on their availability in the ischemic penumbra in the early phase after stroke onset, corresponding to the therapeutic window (<4.5 hours), which is similar in human and experimental stroke. This review summarizes a large body of literature on the spatiotemporal and cellular production of TNF, IL-1, and IL-6, focusing on the early phase in experimental and human stroke. We also review studies of cytokines in blood and cerebrospinal fluid in stroke. Tumor necrosis factor and IL-1 are upregulated early in peri-infarct microglia. Newer literature suggests that IL-6 is produced by microglia, in addition to neurons. Tumor necrosis factor- and IL-1-producing macrophages infiltrate the infarct and peri-infarct with a delay. This information is discussed in the context of suggestions that neuronal sensitivity to ischemia may be modulated by cytokines. The fact that TNF and IL-1, and suppossedly also IL-6, are produced by microglia within the therapeutic window place these cells centrally in potential future stroke therapy.
Figures

Similar articles
-
Interleukin-1beta and tumor necrosis factor-alpha are expressed by different subsets of microglia and macrophages after ischemic stroke in mice.J Neuroinflammation. 2008 Oct 23;5:46. doi: 10.1186/1742-2094-5-46. J Neuroinflammation. 2008. PMID: 18947400 Free PMC article.
-
Electroacupunctre improves motor impairment via inhibition of microglia-mediated neuroinflammation in the sensorimotor cortex after ischemic stroke.Life Sci. 2016 Apr 15;151:313-322. doi: 10.1016/j.lfs.2016.01.045. Epub 2016 Mar 14. Life Sci. 2016. PMID: 26979777
-
Conditional ablation of myeloid TNF increases lesion volume after experimental stroke in mice, possibly via altered ERK1/2 signaling.Sci Rep. 2016 Jul 7;6:29291. doi: 10.1038/srep29291. Sci Rep. 2016. PMID: 27384243 Free PMC article.
-
Potential of anticytokine therapies in central nervous system ischaemia.Expert Opin Biol Ther. 2001 Mar;1(2):227-37. doi: 10.1517/14712598.1.2.227. Expert Opin Biol Ther. 2001. PMID: 11727532 Review.
-
Inflammatory cytokines in acute ischemic stroke.Curr Pharm Des. 2008;14(33):3574-89. doi: 10.2174/138161208786848739. Curr Pharm Des. 2008. PMID: 19075734 Review.
Cited by
-
Adenosine A2A receptor agonist polydeoxyribonucleotide ameliorates short-term memory impairment by suppressing cerebral ischemia-induced inflammation via MAPK pathway.PLoS One. 2021 Mar 18;16(3):e0248689. doi: 10.1371/journal.pone.0248689. eCollection 2021. PLoS One. 2021. PMID: 33735236 Free PMC article.
-
The potential roles of 18F-FDG-PET in management of acute stroke patients.Biomed Res Int. 2013;2013:634598. doi: 10.1155/2013/634598. Epub 2013 May 15. Biomed Res Int. 2013. PMID: 23762852 Free PMC article. Review.
-
Galectin-3 enhances angiogenic and migratory potential of microglial cells via modulation of integrin linked kinase signaling.Brain Res. 2013 Feb 16;1496:1-9. doi: 10.1016/j.brainres.2012.12.008. Epub 2012 Dec 14. Brain Res. 2013. PMID: 23246924 Free PMC article.
-
Mesenchymal stem cell-based treatments for stroke, neural trauma, and heat stroke.Brain Behav. 2016 Aug 3;6(10):e00526. doi: 10.1002/brb3.526. eCollection 2016 Oct. Brain Behav. 2016. PMID: 27781140 Free PMC article. Review.
-
Triptolide Protects Against Ischemic Stroke in Rats.Inflammation. 2015 Aug;38(4):1617-23. doi: 10.1007/s10753-015-0137-x. Inflammation. 2015. PMID: 25687641
References
-
- Allan SM, Tyrrell PJ, Rothwell NJ. Interleukin-1 and neuronal injury. Nat Rev Immunol. 2005;5:629–640. - PubMed
-
- Astrup J, Siesjo BK, Symon L. Thresholds in cerebral ischemia - the ischemic penumbra. Stroke. 1981;12:723–725. - PubMed
-
- Back T, Hemmen T, Schuler OG. Lesion evolution in cerebral ischemia. J Neurol. 2004;251:388–397. - PubMed
-
- Banwell V, Sena ES, Macleod MR. Systematic review and stratified meta-analysis of the efficacy of interleukin-1 receptor antagonist in animal models of stroke. J Stroke Cerebrovasc Dis. 2009;18:269–276. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

