Safety of elective management of synchronous aortic disease with simultaneous thoracic and aortic stent graft placement
- PMID: 22743020
- PMCID: PMC3766713
- DOI: 10.1016/j.jvs.2012.03.272
Safety of elective management of synchronous aortic disease with simultaneous thoracic and aortic stent graft placement
Abstract
Background: Simultaneous treatment of multilevel aortic disease is controversial due to the theoretic increase in morbidity. This study was conducted to define the outcomes in patients treated electively with simultaneous thoracic endovascular aortic aneurysm repair (TEVAR) and abdominal aortic endovascular endografting for synchronous aortic pathology.
Methods: Patients treated with simultaneous TEVAR and endovascular aneurysm repair (T&E) at the University of Florida were identified from a prospectively maintained endovascular aortic registry and compared with those treated with TEVAR alone (TA). The study excluded patients with urgent or emergency indications, thoracoabdominal or mycotic aneurysm, and those requiring chimney stents, fenestrations, or visceral debranching procedures. Demographics, anatomic characteristics, operative details, and periprocedural morbidity were recorded. Mortality and reintervention were estimated using life-table analysis.
Results: From 2001 to 2011, 595 patients underwent TEVAR, of whom 457 had elective repair. Twenty-two (18 men, 82%) were identified who were treated electively with simultaneous T&E. Mean ± standard deviation age was 66 ± 9 years, and median follow-up was 8.8 months (range, 1-34 months). Operative indications for the procedure included dissection-related pathology in 10 (45%) and various combinations of degenerative etiologies in 12 (55%). Compared with TA, T&E patients had significantly higher blood loss (P < .0001), contrast exposure (P < .0001), fluoroscopy time (P < .0001), and operative time (P < .0001). The temporary spinal cord ischemia rate was 13.6% (n = 3) for the T&E group and 6.0% for TA (P = .15); however, the permanent spinal cord ischemia rate was 4% for both groups (P = .96). The 30-day mortality for T&E was 4.5% (n = 1) compared with 2.1% (n = 10) for TA. Temporary renal injury (defined by a 25% increase over baseline creatinine) occurred in two T&E patients (9.1%), with none requiring permanent hemodialysis; no significant difference was noted between the two groups (P = .14). One-year mortality and freedom from reintervention in the T&E patients were 81% and 91%, respectively.
Conclusions: Acceptable short-term morbidity and mortality can be achieved with T&E compared with TA, despite longer operative times, greater blood loss, and higher contrast exposure. There was a trend toward higher rates of renal and spinal cord injury, so implementation of strategies to reduce the potential of these complications or consideration of staged repair is recommended. Short-term reintervention rates are low, but longer follow-up and greater patient numbers are needed to determine procedural durability and applicability.
Copyright © 2012 Society for Vascular Surgery. Published by Mosby, Inc. All rights reserved.
Conflict of interest statement
Author conflict of interest: none.
Figures

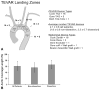

Similar articles
-
Short-term outcomes of the t-Branch off-the-shelf multibranched stent graft for reintervention after previous infrarenal aortic repair.J Vasc Surg. 2020 Nov;72(5):1558-1566. doi: 10.1016/j.jvs.2020.02.012. Epub 2020 May 15. J Vasc Surg. 2020. PMID: 32423775
-
Fenestrated and branched stent-grafting after previous open or endovascular aortic surgery.J Cardiovasc Surg (Torino). 2014 Apr;55(2 Suppl 1):95-103. J Cardiovasc Surg (Torino). 2014. PMID: 24796902
-
Endovascular repair of acute juxtarenal and thoracoabdominal aortic aneurysms with surgeon-modified fenestrated endografts.J Vasc Surg. 2020 Aug;72(2):435-444. doi: 10.1016/j.jvs.2019.10.056. Epub 2019 Dec 25. J Vasc Surg. 2020. PMID: 31882311
-
Systematic review and meta-analysis of published studies on endovascular repair of thoracoabdominal aortic aneurysms with the t-Branch off-the-shelf multibranched endograft.J Vasc Surg. 2020 Aug;72(2):716-725.e1. doi: 10.1016/j.jvs.2020.01.049. Epub 2020 Apr 1. J Vasc Surg. 2020. PMID: 32247700
-
Advanced Endovascular Treatment of Complex Aortic Pathology.Surg Clin North Am. 2023 Aug;103(4S):e1-e11. doi: 10.1016/j.suc.2023.07.008. Epub 2023 Aug 25. Surg Clin North Am. 2023. PMID: 37839825 Review.
Cited by
-
Analysis of Spinal Cord Infarction Associated with Aortic Stent Graft Placement Using Nationwide Inpatient Sample (2002-2011).J Vasc Interv Neurol. 2016 Jan;8(5):9-16. J Vasc Interv Neurol. 2016. PMID: 26958147 Free PMC article.
-
Simultaneous endovascular repairs of concomitant ruptured abdominal aortic aneurysm and huge silent thoracic aortic aneurysm.Indian Heart J. 2016 Sep;68 Suppl 2(Suppl 2):S66-S68. doi: 10.1016/j.ihj.2016.05.009. Epub 2016 May 27. Indian Heart J. 2016. PMID: 27751332 Free PMC article.
-
Thoracic Endovascular Aortic RepairAcutely Augments Left Ventricular Biomechanics in An Animal Model: A Mechanism for Postoperative Heart Failure and Hypertension.Ann Vasc Surg. 2023 Nov;97:18-26. doi: 10.1016/j.avsg.2023.04.007. Epub 2023 Apr 15. Ann Vasc Surg. 2023. PMID: 37068623 Free PMC article.
-
Increased plasma VEGF levels following ischemic preconditioning are associated with downregulation of miRNA-762 and miR-3072-5p.Sci Rep. 2016 Dec 1;6:36758. doi: 10.1038/srep36758. Sci Rep. 2016. PMID: 27905554 Free PMC article.
-
A new method for protection from shower embolism during TEVAR on a shaggy aorta.Gen Thorac Cardiovasc Surg. 2015 Feb;63(2):105-8. doi: 10.1007/s11748-013-0278-5. Epub 2013 Jun 22. Gen Thorac Cardiovasc Surg. 2015. PMID: 23794197
References
-
- Makaroun MS, Dillavou ED, Kee ST, Sicard G, Chaikof E, Bavaria J, et al. Endovascular treatment of thoracic aortic aneurysms: results of the phase II multicenter trial of the GORE TAG thoracic endoprosthesis. J Vasc Surg. 2005;41:1–9. - PubMed
-
- EVAR trial participants. Endovascular aneurysm repair versus open repair in patients with abdominal aortic aneurysm (EVAR trial 1): randomised controlled trial. Lancet. 2005;365:2179–86. - PubMed
-
- Sicard GA, Zwolak RM, Sidawy AN, White RA, Siami FS Society for Vascular Surgery Outcomes Committee. Endovascular abdominal aortic aneurysm repair: long-term outcome measures in patients at high-risk for open surgery. J Vasc Surg. 2006;44:229–36. - PubMed
-
- Aarts F, van Sterkenburg S, Blankensteijn JD. Endovascular aneurysm repair versus open aneurysm repair: comparison of treatment outcome and procedure-related reintervention rate. Ann Vasc Surg. 2005;19:699–704. - PubMed
-
- Lederle FA. Abdominal aortic aneurysm– open versus endovascular repair. N Engl J Med. 2004;351:1677–9. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

