Significance of the balance between regulatory T (Treg) and T helper 17 (Th17) cells during hepatitis B virus related liver fibrosis
- PMID: 22745730
- PMCID: PMC3380028
- DOI: 10.1371/journal.pone.0039307
Significance of the balance between regulatory T (Treg) and T helper 17 (Th17) cells during hepatitis B virus related liver fibrosis
Abstract
Background: Hepatitis B virus-related liver fibrosis (HBV-LF) always progresses from inflammation to fibrosis. However, the relationship between these two pathological conditions is not fully understood. Here, it is postulated that the balance between regulatory T (Treg) cells and T helper 17 (Th17) cells as an indicator of inflammation may predict fibrosis progression of HBV-LF.
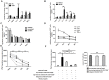
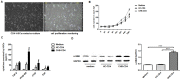
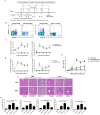
Methodology/principal findings: The frequencies and phenotypes of peripheral Treg and Th17 cells of seventy-seven HBeAg-positive chronic hepatitis B (CHB) patients who underwent liver biopsies and thirty healthy controls were determined by flow cytometry. In the periphery of CHB patients, both Treg and Th17 frequencies were significantly increased and correlated, and a lower Treg/Th17 ratio always indicated more liver injury and fibrosis progression. To investigate exact effects of Treg and Th17 cells during HBV-LF, a series of in vitro experiments were performed using purified CD4(+), CD4(+)CD25(+), or CD4(+)CD25(-) cells from the periphery, primary human hepatic stellate cells (HSCs) isolated from healthy liver specimens, human recombinant interleukin (IL)-17 cytokine, anti-IL-17 antibody and HBcAg. In response to HBcAg, CD4(+)CD25(+) cells significantly inhibited cell proliferation and cytokine production (especially IL-17 and IL-22) by CD4(+)CD25(-) cells in cell-contact and dose-dependent manners. In addition, CD4(+) cells from CHB patients, compared to those from HC subjects, dramatically promoted proliferation and activation of human HSCs. Moreover, in a dramatically dose-dependent manner, CD4(+)CD25(+) cells from CHB patients inhibited, whereas recombinant IL-17 response promoted the proliferation and activation of HSCs. Finally, in vivo evidence about effects of Treg/Th17 balance during liver fibrosis was obtained in concanavalin A-induced mouse fibrosis models via depletion of CD25(+) or IL-17(+) cells, and it's observed that CD25 depletion promoted, whereas IL-17 depletion, alleviated liver injury and fibrosis progression.
Conclusions/significance: The Treg/Th17 balance might influence fibrosis progression in HBV-LF via increase of liver injury and promotion of HSCs activation.
Conflict of interest statement
Figures



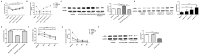
References
-
- Lu FM, Zhuang H. Management of hepatitis B in China. Chin Med J (Engl) 2009;122:3–4. - PubMed
-
- Sakaguchi S, Yamaguchi T, Nomura T, Ono M. Regulatory T Cells and Immune Tolerance. Cell. 2008;133:775–787. - PubMed
-
- Stoop JN, van der Molen RG, Baan CC, van der Laan LJ, Kuipers EJ, et al. Regulatory T Cells Contribute to the Impaired Immune Response in Patients With Chronic Hepatitis B Virus Infection. Hepatology. 2005;41:771–778. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

