Long-term survival from adenocarcinoma of the esophagus after transthoracic and transhiatal esophagectomy
- PMID: 22747995
- PMCID: PMC3476969
- DOI: 10.1186/1477-7819-10-130
Long-term survival from adenocarcinoma of the esophagus after transthoracic and transhiatal esophagectomy
Abstract
Background: The effects of transthoracic or transhiatal esophagectomy on the long-term survival of patients who had adenocarcinoma of the esophagus were compared, as were factors applicable in preoperative stratification of patient treatment.
Methods: A cohort of 147 consecutive patients with adenocarcinoma of the esophagus was evaluated for esophagectomy between 1984 and 2000. The patients were followed prospectively and observed survival rates of patients with a transthoracic or transhiatal approach to esophagectomy were compared by standardized mortality ratio (SMR) and relative mortality ratio (RMR) using the expected survival of a matched Norwegian population.
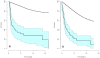
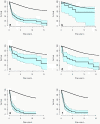
Results: A R0 resection was performed by transthoracic (n = 33) or a transhiatal (n = 55) esophagectomy in 88 (60%) patients with a median age of 61 (range: 35-77) and 70 (42-88) years, respectively (P <0.001). Tumor stages and other possible risk factors were similar in the two groups. Transthoracic or transhiatal esophagectomy resulted in a median survival time of 20.5 (95% confidence interval (CI): 10.4-57.6) and 16.4 (10.6-28.7) months, respectively. The respective survival rates were 31.2% and 27.8% by 5 years, and 21.3% and 16.6% by 10 years with an overall RMR of 1.14 (P = 0.63). Median survival time in the absence or presence of lymph node metastases was 74.0 (95% CI: 17.5-166.4) and 10.7 (7.9-14.9) months. The corresponding survival rates by 10 years with non-involved or involved nodes were 48.9% and 3.8% respectively (RMR 2.22, P = 0.007). Patients with a pT1-tumor were few and the survival rate was not very different from that of the general population (SMR = 1.7, 95% CI: 0.7-4.1). The median survival time of patients with a pT2-tumor was 30.4 (95% CI: 9.0-142) months and with a pT3-tumor 14 (9.2-16.4) months. The survival rates by 10 years among patients with a pT1 tumor were 57.0% (95% CI: 14.9-78.9), pT2 33.3% (11.8-52.2), and pT3 7.1% (1.9-15.5). The relative mortality for T3 stages compared to T1 stages was statistically significant (RMR = 3.22, P = 0.024).
Conclusion: Transthoracic and transhiatal esophagectomy are both effective approaches for treatment of adenocarcinoma of the esophagus and survival of more than 10 years can be expected without adjuvant chemotherapy. However, increasing depth of tumor invasion and lymph node metastases reduce life expectancy.
Figures
References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

