Predictors of first recurrence of Clostridium difficile infection: implications for initial management
- PMID: 22752869
- PMCID: PMC3388024
- DOI: 10.1093/cid/cis356
Predictors of first recurrence of Clostridium difficile infection: implications for initial management
Abstract
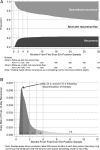
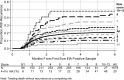
Symptomatic recurrence of Clostridium difficile infection (CDI) occurs in approximately 20% of patients and is challenging to treat. Identifying those at high risk could allow targeted initial management and improve outcomes. Adult toxin enzyme immunoassay-positive CDI cases in a population of approximately 600,000 persons from September 2006 through December 2010 were combined with epidemiological/clinical data. The cumulative incidence of recurrence ≥ 14 days after the diagnosis and/or onset of first-ever CDI was estimated, treating death without recurrence as a competing risk, and predictors were identified from cause-specific proportional hazards regression models. A total of 1678 adults alive 14 days after their first CDI were included; median age was 77 years, and 1191 (78%) were inpatients. Of these, 363 (22%) experienced a recurrence ≥ 14 days after their first CDI, and 594 (35%) died without recurrence through March 2011. Recurrence risk was independently and significantly higher among patients admitted as emergencies, with previous gastrointestinal ward admission(s), last discharged 4-12 weeks before first diagnosis, and with CDI diagnosed at admission. Recurrence risk also increased with increasing age, previous total hours admitted, and C-reactive protein level at first CDI (all P < .05). The 4-month recurrence risk increased by approximately 5% (absolute) for every 1-point increase in a risk score based on these factors. Risk factors, including increasing age, initial disease severity, and hospital exposure, predict CDI recurrence and identify patients likely to benefit from enhanced initial CDI treatment.
Figures

References
-
- Johnson S. Recurrent Clostridium difficile infection: a review of risk factors, treatments, and outcomes. J Infect. 2009;58:403–10. - PubMed
-
- Aslam S, Hamill RJ, Musher DM. Treatment of Clostridium difficile-associated disease: old therapies and new strategies. Lancet Infect Dis. 2005;5:549–57. - PubMed
-
- Garey KW, Sethi S, Yadav Y, DuPont HL. Meta-analysis to assess risk factors for recurrent Clostridium difficile infection. J Hosp Infect. 2008;70:298–304. - PubMed
-
- Pepin J, Alary ME, Valiquette L, et al. Increasing risk of relapse after treatment of Clostridium difficile colitis in Quebec, Canada. Clin Infect Dis. 2005;40:1591–7. - PubMed
-
- Hu MY, Katchar K, Kyne L, et al. Prospective derivation and validation of a clinical prediction rule for recurrent Clostridium difficile infection. Gastroenterology. 2009;136:1206–14. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

